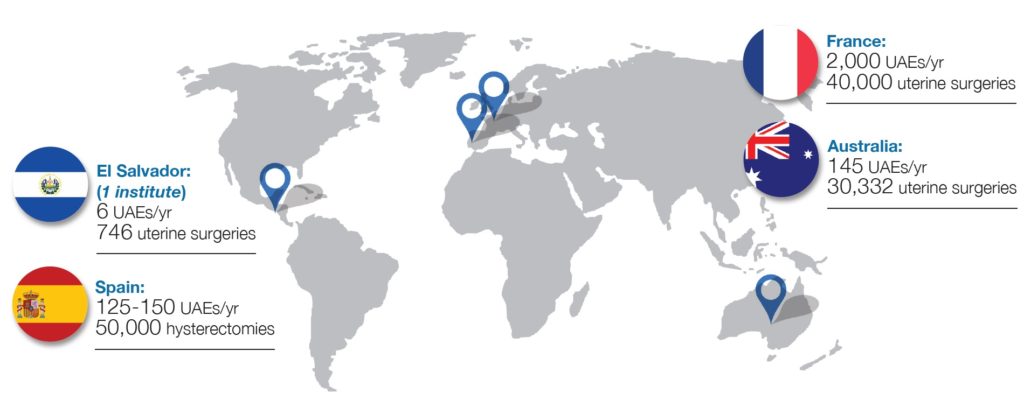
On average in France, 2,000 uterine artery embolizations (UAEs) are performed each year. In contrast, 40,000 patients have hysterectomies annually. This has led French interventional radiologists to protest the high number of “unnecessary” surgeries, and spurred the development of a nation-wide public awareness campaign. However, this is not just a French issue.
James Spies (Georgetown University Hospital, Washington, DC, USA) reports that, “despite some progress in reducing the number of hysterectomies for benign conditions such as fibroids, with about a 10% reduction in the past decade, there are still eight to 10 times the number of hysterectomies as UAEs for fibroids in the USA.”
A 2017 report by the Society of Interventional Radiology (SIR), The Fibroid Fix: What women need to know, provided insights into the lack of awareness. SIR commissioned a Harris Poll in June 2017 that surveyed 1,176 US women ages 18 and over. The poll found 62% of respondents had never heard of UAE and that 20% believed hysterectomy was the only treatment option for fibroids. Even those who were diagnosed with fibroids reported a lack of awareness, with 44% saying they had not heard of UAE. Of those who had, 75% said they did not learn about it from a gynaecologist.
“Our numbers for UAE are ridiculous,” José Urbano (Ramon y Cajal University Hospital, Madrid, Spain) says of Spain. According to the Spanish Society of Vascular and Interventional Radiology (SERVEI), 120–150 UAE are performed each year in the country, which has a population of 44 million. These experiences are echoed in Central America. Speaking at SIR’s annual meeting last year (23–28 March, Austin, USA), the only interventional radiologist in El Salvador, Ethel Rivas Zuleta (Universidad Dr José Matías Delgado, San Salvador, El Salvador), told delegates: “We face the same problems in our region”. Fibroids are the leading indication for hysterectomy in El Salvador. In 2018, 746 hysterectomies were performed in Zuleta’s institution, mostly in women between 30 and 50 years of age. Six women were treated with UAE. Zuleta noted that none of these six patients were referred by an obstetrician or gynaecologist: four were either doctors themselves, or related to one, and two had found out about UAE themselves online.
On the other side of the world, Gerard Goh (The Alfred Hospital, Melbourne, Australia) and colleagues recently analysed Australian Medicare data, and found a “huge disparity” between the number of hysterectomies performed each year compared with the number of UAEs. The data showed that, on average over the last five years, 30,332 uterine surgeries are performed each year. According to Goh, you would expect four to five thousand of these (approximately 30%) to be treatment for fibroids. Fewer than 145 UAEs were performed on average per year. “Based on the suggestion that 20% of hysterectomies in Australia are for fibroid-related disease, this estimates 6,066 fibroid-related surgeries per year,” Goh comments.
He adds that he thinks it is “interesting” that a procedure which has been proven to be efficacious has such a poor take-up globally. A major reason for this, he posits, is the lack of “patient and referrer awareness”. To tackle this issue, he believes interventional radiologists from across the world need to “come together” and work with societies to help educate patients and referrers, because currently “a lot of women are really missing out on uterus-sparing surgery for fibroids”.
Why this discrepancy?
Speaking specifically of the US population, Spies expands on his thoughts for the causes of the discrepancy between hysterectomy patient numbers and UAE patient numbers: “I believe that there are a range of factors, which could include economic considerations, but also persisting scepticism among gynaecologists about UAE. Despite considerable evidence of excellent outcomes after UAE, UAE patients are more likely to need additional interventions than those that have hysterectomy and many gynaecologists seem convinced that a definitive treatment like hysterectomy is best. [However, we must take into account] women’s desire to avoid hysterectomy.
“In the USA, we have made efforts for years to raise the profile of UAE, with some success. Still, it is an effort of decades that will cause change. Currently, SIR is engaged in a multi-disciplinary creation of practice guidelines for the procedure.”
These guidelines, which are expected to be published in early 2021, are being developed by physicians from the specialties of gynaecology, body imaging, and IR. “The guidelines will amplify SIR’s past awareness and education efforts by providing physicians and patients with evidence-based recommendations for the optimum care of patients with symptomatic fibroids,” SIR president Laura Findeiss (Grady Memorial Hospital, Emory University School of Medicine, Atlanta, USA) comments.
In addition to SIR, the participating societies are Cardiovascular and Interventional Radiological Society of Europe (CIRSE), Fédération Internationale de Gynécologie et d’Obstétrique (FIGO), the American Association of Gynaecologic Laparoscopists (AAGL), the American Society for Reproductive Medicine (ASRM), and the Society for Advanced Body Imaging (SABI).
To attract a Medicare rebate for UAE in Australia, the patient must be referred by an obstetrician/gynaecologist, which Goh says “brings up potential referral bias”. However, he notes that the low UAE rate in Australia is “likely multifactorial”, and that IR can only fulfil its potential in terms of treating the appropriate number of eligible patients when interventional radiologists “take greater clinical ownership of their patients”. To Goh, this looks like preprocedural consultations with patients, postprocedural care, and having an inpatient bed card. He also stresses that gynaecologists and interventional radiologists alike should have an understanding of the pros and cons of both embolization and surgical options, to allow patients to make an informed decision about their fibroid treatment.
Urbano concurs with Goh’s assessment that there are numerous reasons for the underutilisation of UAE globally, and particularly in Spain. “Of course, like in France, gynaecologists actively block this treatment because they fear losing patients,” he says. “Furthermore, when obtaining informed consent for hysterectomy, it is mandatory to notify the patient that UAE is offered as an alternative, but it is often not even mentioned. Gynaecology tends to be a speciality that does not participate in multidisciplinary work. They have countless patients, they do their own diagnostic tests, and their patient management is routine.
“Interventional radiologists have too much work in Spanish public hospitals, so UAE is not an important focus for them. In addition, while they are experts at doing the procedure, they are not always involved in the diagnosis, pain management, and patient follow-up. Interventional radiologists are only fully involved in the UAE process in private practice and some public hospitals. Less than 50% of IR services in Spain have a clinic and beds. In my experience, this is crucial for us to do all those type of procedures in which IR competes with other specialties.”
Zuleta argues the same in El Salvador. She says the underutilisation of UAE is due to “a lack of knowledge by other specialties, the usage of old protocols and guidelines, and highly unequal access to healthcare for women. We do have access to technology: we have angiosuites, CTs, ultrasounds, MRI, but what we lack is education. We at SIDI [Sociedad Iberoamericana De Intervencionismo] believe that supporting education in our countries is the best way to improve the management of patients, especially in IR.”
Public awareness initiatives
In the USA, SIR is running its own campaign—the Vision to Heal, Together, launched in September 2019—to bring IR procedures to the forefront of the public consciousness. According to an SIR press release, this aims to “build stronger partnerships with referring physicians and to empower patients to ask about IR as a treatment option.” The campaign is not specific to UAE, it is focused more broadly on vascular disease, cancer, and men’s health conditions, which includes uterine fibroids. SIR is using a combination of radio, digital, and social media advertising in four pilot US markets (Washington, DC; Rochester; Little Rock; Portland) to spread its messaging.
The campaign was inspired in part by SIR’s 2017 report finding the lack of awareness among patients and the lack of information from referring physicians. “By educating both groups, we hope to not just reduce the knowledge gap, but to build trust among the specialties so that patients are presented with all of their treatment options up front,” says Findeiss.
The Vision to Heal, Together campaign ran through to the end of March 2020. SIR reports positive engagement and social media posts. “We have seen friends sharing information with friends in need and others simply commenting to vouch for the life-saving and quality-of-life improving power of interventional radiology,” Findeiss comments. “There is a real desire and need for more information about minimally invasive treatments across the board.”
In Australia, the wording of the Medicare item for UAE is under review, which Goh hopes will change to improve patient access to the procedure. The Interventional Radiology Society of Australasia (IRSA), of which Goh is president, is “working on the UAE issue.” Goh says: “We are working with some other stakeholders to increase public awareness online, and via print and social media.” IRSA is updating its website to list practitioners who can perform UAE, and is leading a global position statement to help further increase awareness.
In Spain, Urbano stresses that the key lesson from the French action is that it is patient-focused. “SERVEI’s position is not to start turf battles,” he says. “We have lost too much time and energy in the past with no-way fights. Our policy is to show what IR work is, and to demonstrate he advantages of our treatments to patients.”













