 This advertorial is sponsored by Guerbet. SeQure®
This advertorial is sponsored by Guerbet. SeQure®
As the leader of an investigator-initiated, Phase 2 study evaluating the safety and efficacy of the SeQure® microcatheter (Guerbet), Francisco Cesar Carnevale here outlines his experience using the device, drawing particular attention to the reduced risk of reflux and non-target embolization. Originally scheduled to be presented at the Society of Interventional Radiology (SIR) Annual Scientific Meeting, this early experience with the SeQure® microcatheter in prostate artery embolization (PAE) is promising, with Carnevale hopeful it will enable the delivery of more therapeutics to the target vessel, while reducing damage to healthy tissue.
PAE is a novel, minimally invasive treatment for lower urinary tract symptoms (LUTS) attributed to benign prostate hyperplasia (BPH). Embolization of the prostatic arteries leads to ischaemic shrinkage of the prostate gland and subsequent reduction of LUTS. PAE’s therapeutic effect was first described in a case report in 2000. The first intentional treatment of BPH in humans was reported in 2010, and early cohort studies from around the world soon followed.
As with any new treatment, there is a learning curve. The more cases we perform, the more apparent it becomes to us that making even minor changes to our technique can make a difference to the outcome. One of the main concerns regarding PAE is related to non-target embolization (NTE). This is often due to one of three main causes: (A) reflux of embolic agents around the microcatheter into the main artery that feeds the prostatic artery (types I–V from the University of São Paulo Classification); (B) reflux or flow-direct injection of embolic agents to proximal, non-target branches; and (C) distal injection of embolic agents through intraprostatic shunts. The most common regions to NTE are the bladder, seminal vesical, rectum, penis, and pubic bone. So, having a refined technique and using dedicated microcatheters are key to a good and safe embolization.
With the aim of identifying a microcatheter that reduces the risk of NTE and which could be used as an alternative option, we have initiated the first PAE clinical study using the SeQure® microcatheter at the University of São Paulo Medical School (Prostate Artery Embolization using the SeQure® Microcatheter: A Phase 2 Study Addressing Safety and Efficacy).
The main goals of this microcatheter are to reduce the risk of reflux and NTE, and deliver more therapeutics to the target vessel while reducing damage to healthy tissue. Observations from our early experience—we have performed three procedures—indicate that PAE can be safely and effectively performed with the SeQure® microcatheter, even when navigating distally using the PErFecTED technique.
Case 1
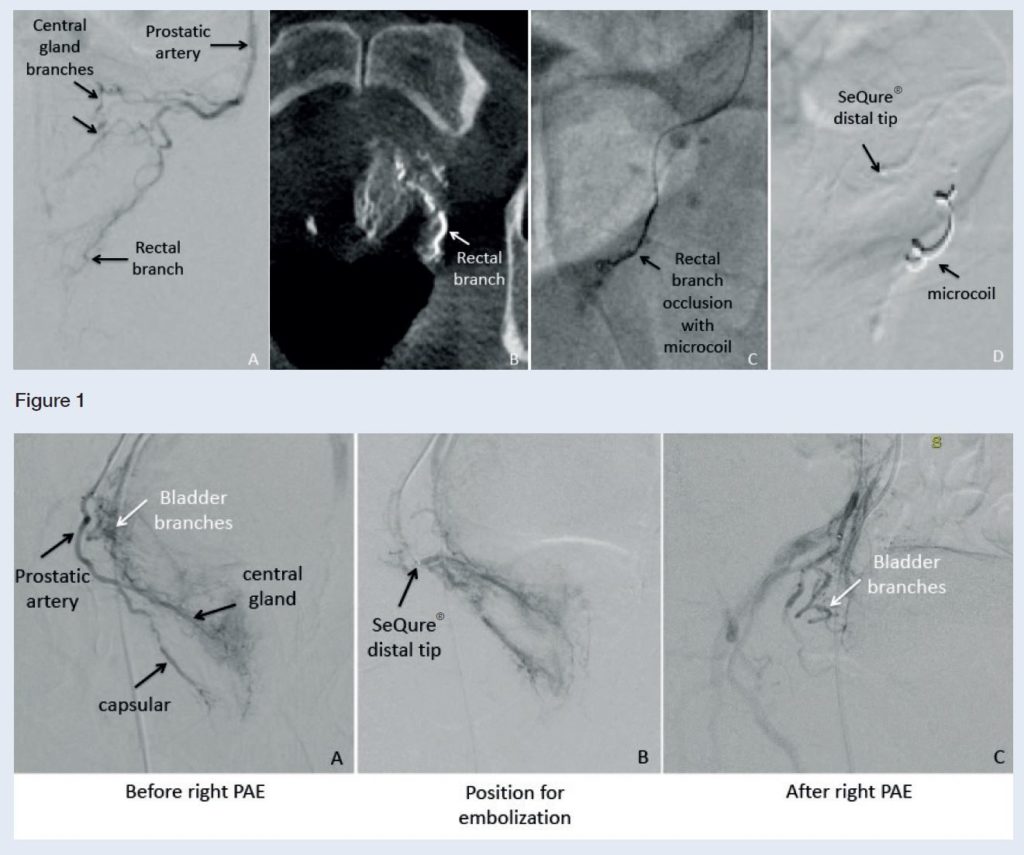
A 70-year-old man with IPSS: 33 (nocturia 4x, weak urinary stream, incomplete voiding, frequency and intermittence). QoL: 6; PSA: 1.40 ng/mL; Qmax: 4.10 mL/sec; prostate volume by MRI: 70 grams; post-void residual volume by US: 40 mL. The patient was refractory to LUTS medication (taken for decades already) and PAE was chosen over surgery to avoid the risk of complications, mainly because of his age. To avoid NTE into the rectal branches—shown by digital subtraction angiography (DSA; Figure 1A) and cone beam computed tomography (CBCT; Figure 1B)—the SeQure® microcatheter was placed distally at the capsular branch, closing the communication with a metallic microcoil (Figure 1C). After injecting the embolic agents from the proximal position (before the bifurcation into the central gland and peripheral zone branches), the SeQure® microcatheter was easily navigated deeply into the central gland branch (Figure 1D) to inject additional particles according to the PErFecTED technique.
Case 2
A 65-year-old man with IPSS: 25 (nocturia 3x, urgency, frequency and weak urinary stream). QoL: 5; PSA: 3.40 ng/mL; Qmax: 6.50 mL/sec; prostate volume by MRI: 46.5 grams; postvoid residual volume by US: 5 mL. Refractory to LUTS medication after taking it for several years; PAE was chosen to avoid the risk of complications, and upon the recommendation of a friend of the patient previously treated with PAE.
During DSA of the right prostatic artery, some bladder branches were identified before the origin of the central gland and the capsular branches (Figure 2A). The SeQure® microcatheter was advanced distally to the bladder branches and positioned before the bifurcation of the central gland and capsular branches for a safer embolization (Figure 2B). One of the risks and consequences when performing this embolization step is the occlusion (NTE) of bladder branches proximal to the prostate resulting in bladder ischaemia. The side slits on the 1 cm distal tip of the SeQure® microcatheter allow the outflow of contrast media without passage of the embolic agent, meaning the bladder branches were saved from NTE (Figure 2C).
We hope that the data obtained from this important study will help bring a new, exciting device to those in the medical community performing this technically challenging procedure. Interventional radiologists should adopt a strategic, multidisciplinary approach to develop pre-clinical and clinical research, and to ultimately transfer current evidence into clinical practice.
Francisco Cesar Carnevale is the director of Vascular Interventional Radiology at the University of São Paulo Medical School, Sao Paulo, Brazil. He has received consulting and speaker honoraria from Guerbet.
Results from case studies are not necessarily predictive of results in other cases. Results in other cases may vary.











