Many regulatory jurisdictions are establishing different approaches for medical devices, Misti Malone, assistant director in the Office of Cardiovascular Devices at the US Food and Drug Administration (FDA) said recently at the 2019 Vascular and InterVentional Advances meeting (VIVA; 4–7 November, Las Vegas, USA). She talked the audience through recent regulatory changes across the world, and outlined her vision for a global regulatory consensus.
Speaking in the “Most controversial clinical challenges of 2019” session at VIVA, Malone joked, “I hope you do not consider the FDA the most challenging and controversial aspect of clinical care” as she took to the podium to deliver her talk “Shifting worldwide regulatory priorities: How will changes in the 510(k) and CE mark process affect device availability for patients?”
“We [the FDA] are here to interact and collaborate with you,” she told the physicians, “and we appreciate the hard work you are doing. […] Regulatory pathways are evolving across the world. While I was asked to comment on whether this may affect device availability, our primary mission is to promote and protect public health, and our goal is to bring safe and effect devices to patients. We try to do this as quickly as possible, so we hope that our pathways are not changing how devices are available, other than potentially making devices available more quickly, and as needed by some of our new pathways.”
While she detailed how many regulatory jurisdictions are establishing different regulatory approaches for medical devices, exploring the changes to the FDA pathways in the US, she urged the VIVA audience to consider global strategies when appropriate. “We [the FDA] highly recommend discussing these proposals with multiple regulatory agencies early in the process,” she counselled, “so they can be efficient and predictable”.
The FDA 510(k) pathway
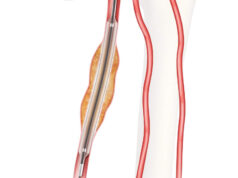
The FDA’s 510(k) pathway is required for most medium-risk devices, classified as Class II by the agency. These include guidewires, introducers, balloon catheters, and peripheral atherectomy devices. Approval via this pathway requires the demonstration of “substantial equivalence to a legally marketed, predicate device”, meaning that the new device design, performance, and intended use must be similar enough to an existing device.
On 20 September 2019, the FDA released a guidance document outlining a new “safety and performance-based pathway”, representing an alternative to the 510(k) process. According to Malone, the clearance was based on the intended use being equivalent to the predicate, and performance testing following FDA-specified methods and criteria, which may be based on recognised standards and the historical performance of comparable products, rather than testing intended to demonstrate substantially equivalent performance to a specific marketed device via methods selected by the manufacturer.
However, Malone acknowledged that this new 510(k) pathway may not be suitable for all devices: “Due to the lack of comprehensive standards and guidances available, particularly for cardiovascular devices […], identifying performance criteria and placing devices in a box may be challenging. Our goal is not to reduce innovation—it is to support innovation by allowing the process to move as efficiently as possible.”
One of the goals of this new pathway, Malone shared, is to make the approval process in the USA “more similar to regulatory paradigms in other countries”, such as the third party certification in Japan, which relies on performance criteria set by the Japanese government. As this only includes a limited number of cardiovascular devices, Malone anticipated that “This [system in Japan] may be pathway that will be valuable for some of our simpler devices for which we can set our performance criteria, but not for all devices.” She was enthusiastic, though, about the potential for global regulatory synergy, commenting: “It may facilitate convergence for global regulatory decision-making.”
EU MDR changes will take effect from May 2020
The European Union is moving to replace its Medical Device Directive (MDD) with the Medical Devices Regulation (MDR), a more extensive regulatory document, introducing significant revisions to quality and safety standards, and the range of regulated devices. The MDR was initiated in May 2017, and a three-year transition period applies. The changes outlined in the MDR legislation are currently due to take effect from May 2020, though, as Malone pointed out, “There is continual discussion on the topic at these forums [referring to meetings like VIVA] and from the EU”.
The goals are to reinforce provisions for clinical evidence. Clinical evaluation will be required pre-market for some devices and modifications, and it will continue into post-market with regular updates, surveillance, and analyses. Another goal is to encourage transparency, using unique device identification (UDI) traceability and data availability for both clinicians and patients. “We hope that this will provide more information, or at least that the EU will provide more information to support clinical decision-making and patient decision-making,” Malone stated.
One worry she shared with the VIVA audience was that clinical data may be required, and that this may affect device availability. Devices that are most likely to require clinical investigation are those that are implants and high-risk devices, those assigned to Class II, low-risk devices where the technology has little or no experience, or devices that extend the intended purpose of an existing technology, Malone informed delegates. For devices classified as Class III and implantable devices, a post-market clinical follow-up report may be required to update a summary of safety report, and clinical performance needs to be updated at least annually with these data.
“How this will affect device availability I think is more of a question for industry,” Malone opined. “I think it may be based on their cost-analysis. However, we look to clinicians to help us understand the ramifications of some of the regulatory decisions, and also to develop a global consensus, so the process can be efficient.”
Harmonising global regulatory requirements
“We have global groups, such as the International Medical Device Regulators Forum, in which we cooperate with numerous countries across the globe,” Malone said. This is a voluntary effort among medical device regulators to, in Malone’s words, “harmonise various regulatory requirements across their jurisdictions. The goal”, she elaborates, is “to be transparent and predictable, and create a reliable pathway, that is efficient for industry, clinicians, and regulators. It is currently high-level, but it is driving cooperation at the device level.”
The FDA and the Center for Devices and Radiological Health (CDRH)—the branch of the FDA responsible for the premarket approval of all medical devices—consider it a strategic priority to use opportunities and collaborations like IMDRF to put in place building blocks for creating a medical device single review programme with the potential goal that, once established, market authorisation and decision in one place may be supported in another country.
The clause in the 2018–2020 CDRH strategic priorities document, published January 2018, outlining how this may work reads: “We also will explore international convergence of some of these pathways—but not change our regulatory standard for market authorisation nor our reliance on valid scientific evidence—as we continue to work under the auspices of the International Medical Device Regulators Forum to put in place the building blocks for creating a Medical Device Single Review Program. Under such a programme, should it be established, the market authorisation decision made by or on behalf of one participating jurisdiction would be relied on wholly or in part to support marketing authorisation by other participating jurisdictions.”
Malone drew the audience’s attention to Japan as a case study of international collaboration. She described a successful harmonisation between the USA and Japan: “The USA collaborates closely with Japan due to the similar regulatory environments and patients. They [Japan] have made some recent policy developments, including [the] Sakigake (pioneer) device scheme, shifts in pre- and post-market balance, similar to the FDA, the use of non-domestic data, establishment of registries and use of real-world evidence, and pathways for early feasibility studies. We have continuing US and Japanese collaboration via HBD [harmonisation by doing].”
HBD facilitates the cooperation of industry, government, and academia in Japan and the USA to align medical device regulations in both countries through clinical trials and the approval review process.