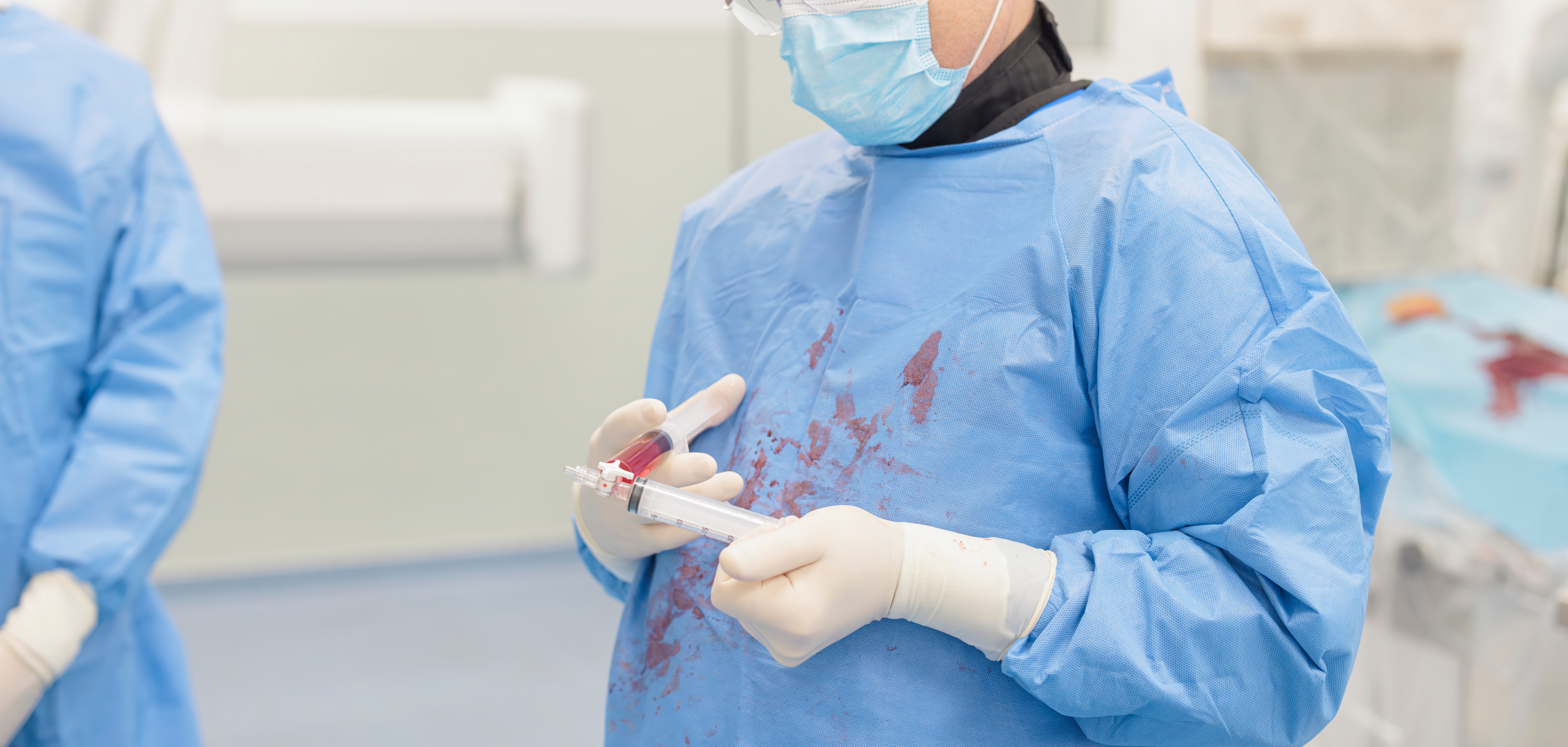
There are substantial differences amongst guideline recommendations regarding the use of prostate artery embolization (PAE) in the treatment of lower urinary tract symptoms/benign prostatic obstruction (LUTS/BPO), which can be partially explained by different interpretation of the evidence. This is the conclusion presented by Dominik Abt (Klinik für Urologie, Institut für Medizin, Universität St Gallen, St Gallen, Switzerland) at the Global Embolization and Cancer Symposium Technologies (GEST) 2021 Focus Day on prostate artery embolization (PAE; 6 March, online). This virtual meeting sought to open discussion between urologists and interventional radiologists regarding the place of PAE in the treatment algorithm, a topic of heated debate in recent years.
Speaking during the final session of the day, panel chair and co-course organiser Jafar Golzarian (University of Minnesota, Minneapolis, USA) praised the “unique” collaborative attitude of the virtual meeting, where attendees heard from four urology panellists and four interventional radiology (IR) panellists: “This session exploring the level of evidence and directions for future research in PAE is unique in both the IR and urology communities,” he said, “taking a truly interactive and multidisciplinary approach, which is not common practice.” He noted that he hoped this cross-disciplinary collaboration would continue in future meetings.
The American Urological Association (AUA) does not recommend PAE for the treatment of LUTS/benign prostatic hyperplasia (BPH) outside the context of a clinical trial, a recommendation attributed to the expert opinion of a panel of urologists. This news was unwelcome to the IR community when first announced in 2019, as interventional radiologists have been advocating for the procedure’s acceptance by the wider medical world. Multiple IR societies conclude that PAE is a safe, effective, minimally invasive treatment option in select BPH patients.
Evidence for PAE

Speaking first, Mark Little (Royal Berkshire NHS Foundation Trust, Reading, UK) discussed the most important PAE articles published in the last two years. In the last two years, 113 papers on PAE have been published. Of these, five were randomised controlled trials (RCTs), and eight were meta-analyses of systematic reviews.
Regarding the clinical effectiveness of PAE, Little said: “We cannot go beyond the superb sham RCT study that came out of Lisbon.” This was a 2019 study published in European Urology, the official journal of the European Association of Urology (EAU), from João Pisco, Tiago Bilhim (Hôpital Saint-Louis, Lisbon, Portugal) et al that found that the improvements in quality of life measurements and International Prostate Symptom Score (IPSS) in patients following PAE are “far superior” to those due to the placebo effect. Speaking to Interventional News at the time, Bilhim noted that publishing a paper positively describing PAE in a urology journal has historically been difficult for interventional radiologists. He hoped that this publication “might help our way into the urology guidelines with PAE”.
“Anyone who has tried to design a sham trial—which I am trying to do now for genicular artery embolization [GAE]—knows that it is hard work,” Little commented, in praise of the Lisbon group. “On the one hand it is the gold standard study design to refute the placebo effect, but there are a number of ethical dilemmas. So it is an ambitious study design, and one that the Lisbon group did extremely well to set up and running and recruit to.”
In the sham study in question, 80 patients were enrolled, randomised 1:1 to PAE versus a sham procedure with a cross-over design at six months. Summarising their findings, Little relayed: “They found a statistically significant refutation of the placebo effect—PAE does better than sham”. Asking the question, “Is PAE clinically effective”, Little argued that the answer was a definitive “Yes”, based off this Level 1 evidence.
Giving a more practical perspective, Little then turned to covering the evidence for altering clinical practice, focusing on papers dedicated to patients with median lobes and to the question of repeat PAE.
“I remember having conversations at CIRSE [the annual scientific meeting of the Cardiovascular and Interventional Radiological Society of Europe] five or so years ago saying ‘Well, perhaps we should exclude patients with a median lobe, they seem to be difficult to treat’,” he said. Presenting a 2019 publication from Riad Salem (Northwestern University, Chicago, USA) and colleagues in Abdominal Radiology, looking predominately at imaging correlates: “A simple study,” Little opined, “but nevertheless [it] gives the idea and the introduction of where we sit with regard to the technique of embolizing the median lobe.” This cohort study showed that 37% of patients had a median lobe—intravesical prostatic protrusion (IPP)—and that 100% of those IPP-positive patients treated with PAE had a decrease in median lobe size following the procedure.

While this demonstrated that it was feasible to embolize the median lobe, Little asked “What does that mean clinically, do these patients get better?” He turned to a 2021 study from GEST co-founder Marc Sapoval, first author Tom Boeken (both Hôpital Européen Georges-Pompidou, Paris, France) et al that concluded that IPP is “not a prognostic marker of ineffective PAE in men with benign prostatic hyperplasia (BPH)”. Sapoval, Boeken and colleagues also wrote that severe protrusion could lead to a better response to PAE, “though expected prostate height reductions are mild”. They found that the degree of IPP did not limit the efficacy of PAE in patients with lower urinary tract symptoms (LUTS) due to BPH.
Furthermore, a 2020 paper in the Journal of Vascular and Interventional Radiology (JVIR) from Aaron Fischman (Mount Sinai, New York, USA) and colleagues answered the direct question “Should we be treating median lobes?”, Little reported. Stratifying the median lobes by size (patients were categorised as having non-severe IPP if their median lobe was <10mm, as was the case in 17 patients enrolled in the study, and as having severe IPP if their median lobe was >10mm, as was the case in 37 patients), Fischman et al found that both groups had a statistically significant improvement in IPSS and quality of life scores. “So we should not be scared of median lobes in terms of PAE,” Little concluded.

Concentrating on repeat PAE, Little relayed how approximately 20% of PAE patients could be deemed “clinical failures”, in need of further intervention. “Does that mean one in five need surgery?” he asked. Again turning to work from the Lisbon group, which focused on how these patients failed, Little recounted how patients in the study were categorised into two groups: group A (n=39), those who never showed a response to PAE; and group B (n=69), those who had clinical improvement in the first six months following PAE, but then relapsed. The investigators found that in 75% of patients, the blood flow was coming from the previously embolized prostate artery, perhaps indicating under-treatment, while in the remaining 25% of patients, the blood supply was from collateral vessels. At 24–26 months follow-up, 17% of group A had a clinical benefit from repeat PAE. This led Little to comment: “Effectively, if you have got a patient that does not respond initially, they are unlikely to respond. They [those in group A] probably need to be treated with surgery.” In group B, meanwhile, 52% had a significant clinical benefit from repeat PAE.
AUA guidelines
 Little also considered the Society of Interventional Radiology (SIR) consensus panel conclusions, which were the focus of much of the day’s discussion. Published in JVIR and authored by Clifford Davis (College of Medicine and Radiology, University of South Florida, Tampa, Florida) et al, the summary of the SIR consensus panel on PAE regarding the development of a research agenda for the procedure concluded without direction: “Level 1 data are required to be included in the AUA guidelines for treatment of BPH. Because of concerns with all three study designs, the panel did not reach a consensus. Further meetings are planned with the panel to select among these research designs.”
Little also considered the Society of Interventional Radiology (SIR) consensus panel conclusions, which were the focus of much of the day’s discussion. Published in JVIR and authored by Clifford Davis (College of Medicine and Radiology, University of South Florida, Tampa, Florida) et al, the summary of the SIR consensus panel on PAE regarding the development of a research agenda for the procedure concluded without direction: “Level 1 data are required to be included in the AUA guidelines for treatment of BPH. Because of concerns with all three study designs, the panel did not reach a consensus. Further meetings are planned with the panel to select among these research designs.”
The three research designs mentioned were: i) RCT of PAE versus sham with crossover of the sham group. (ii) RCT of PAE versus simple prostatectomy. (iii) RCT of PAE versus holmium laser enucleation of the prostate/thulium laser enucleation of the prostate.
The SIR consensus panel ultimately recommended a non-industry-funded registry to obtain real-world data.
Currently, the AUA guidelines state that “PAE for the treatment of LUTS secondary to BPH is not supported by current data and trial designs, and benefit over risk remains unclear; therefore, PAE is not recommended outside the context of clinical trials.” The guidelines claim this advice is based on expert opinion.
“I am a UK interventional radiologist,” Little acknowledged, “so I will be as objective as I can be in this argument.” He talked the GEST audience through the guidelines from the perspective of the SIR consensus paper. He noted that the AUA guidelines included RCTs with more than 12 months of outcome data, but that the AUA wanted PAE studies to include a 24-month follow-up “to be equivalent to current data on other surgical therapies for LUTS resulting from BPH”.
Citing a 2020 JVIR study from Iñigo Isausti (Complejo Hospitalario de Navarra, Pamplona, Spain) et al, Little related how the group set out to compare clinical and functional outcomes of PAE with those of transurethral resection of the prostate (TURP) for the treatment of LUTS secondary to BPH. Isausti and colleagues reported: “Reduction of LUTS in the PAE group was similar to that in the TURP group at 12 months, with fewer complications secondary to PAE.”
However, AUA require two-year data. “We are very fortunate to have Dominik [Abt] here,” Little said, “as the lead author of this paper”. Abt (Klinik für Urologie, Institut für Medizin, Universität St Gallen, St Gallen, Switzerland) et al conducted a study comparing the efficacy and safety of PAE and TURP in the treatment of LUTS at two-year follow-up.
They concluded in February 2021: “Inferior improvements in LUTS/BPO [benign prostatic obstruction] and a relevant re-treatment rate are found 2 years after PAE compared with TURP. PAE is associated with fewer complications than TURP. The disadvantages of PAE regarding functional outcomes should be considered for patient selection and counselling.” Their patient summary was: “PAE is safe and effective. However, compared with TURP, its disadvantages regarding subjective and objective outcomes should be considered for individual treatment choices.”
As the reintervention rate was 20% in the PAE group, Little said what treatment these patients should get next is “where the debate now lies”.
“I do not think this paper is a death knell for PAE at all,” he opined. “Actually, I think it shows that it is safe and effective, but, we need a reasonable discussion with our patients about what we can achieve with the technology based on patient selection, anatomy selection, pre-procedural imaging and planning.”
He concluded that PAE is safe and effective, and, in his eyes, gives patient’s a choice, which he believes is “really important”. Citing the sham trial and RCT data to two-years follow-up, Little summarised that there is “lots of level 1 and 2 evidence on PAE, which cannot be argued against in terms of the position statement of ‘Benefit over risk remains unclear’ [from the AUA guidelines].”
He continued: “I am not sure that we can say that with the current evidence case we have,” something fellow panellist and interventional radiologist Riad Salem (Northwestern Memorial Hospital, Chicago, USA) said he agreed with.

Going through the AUA guidelines comparing how PAE was assessed compared to alternative therapies, James Spies (MedStar Georgetown University Hospital, Washington, DC, USA) said he thought the recommendation not to perform the procedure outside of clinical trials was “actually a value judgement of one specialty of another” that “seems a little unusual”.
“This is not pointing fingers at the AUA,” he added. “I was former chair of the standards committee of the SIR, and I am a former [SIR] president—clinical practice guidelines really are intended to be evidence-based, and by-and-large they are. The process the AUA use is actually very good. But when it gets down to it, it is difficult to separate our preconceived notions from our review of evidence.”
“Again, this is not a knock on the AUA, but my opinion is that guidelines reflect the opinions of the organisations that create them. That is because it is almost impossible for a group in a room to go beyond what is not comfortable for them. In some ways, the SIR is never going to write a guideline that says PAE is bad, probably, unless we have some definitive data, and the AUA may never write one that says it is good or at least should be on the list. So I would agree we need to increase our data, but I am just not sure we are ever going to be able to get there. This is a benchmark procedure for urologists, and, just like some other specialties that we work with, it can be difficult to get adoption.”
When thanking Spies for his talk, Golzarian noted that Spies is a “pioneer” for uterine fibroid embolization (UFE), a procedure now widely recognised and performed by interventional radiologists: “It is like revisiting history; we are 15 years behind with PAE [compared to UFE], but hopefully we will see the same acceptance,” he commented.
Quality of evidence for PAE: The urologist perspective
Speaking next, urologist Philipp Dahm (Minneapolis VA Medical Center and University of Minnesota, Minneapolis, USA) gave a talk entitled, “Objective rating of evidence: Why it matters and how it applies to PAE”. He recommended the following: “Current best evidence on PAE should be assessed on the basis of a high-quality, protocol-driven systematic review. The focus should be on patient-important outcomes with explicit consideration of clinically important differences [in the case of PAE, this includes IPSS and quality of life scores, adverse events, and retreatment rates; flow rate and prostate volume are deemed “not important for decision-making” by Dahm]. The certainty of evidence rating should be provided on a per outcome basis to qualify how much confidence we have. Lastly, judgements about net benefit need to consider both relative and absolute effect size estimates.”
Dahm is a founding member of the US grading of academic assessment, development, and education (GRADE) network, an informal working group formed in 2000 to develop a new system for rating the certainty of evidence in healthcare and also for making guidelines. Currently, GRADE has over 500 members, and is used by more than 120 organisations.
Unlike the traditional “hierarchy of evidence”—which treats systematic reviews, meta-analyses, and randomised controlled trials at the gold standard—GRADE is based on an alternate hierarchy that Dahm said reflects the flaws in these assessment methods. In particular, he noted that RCTs “can be fatally flawed” in their design, and noted that systematic reviews are only as good as the individual studies they evaluate, so could suffer from a “garbage in, garbage out” scenario. In the GRADE system, systematic reviews are “undocked” from the very top of the triangle in the traditional hierarchy of evidence graphic, and are used as a tool for assessing a body of evidence.
The GRADE system works thus: formulate a question; select outcomes; rate the importance of these outcomes (on a scale from critical, to important, to less important) look at outcomes across studies; create an evidence profile with GRADEpro, which includes a summary of findings and an estimate of the effect for each outcome; rate the quality of evidence for each outcome (from high, through moderate and low, to very low).
“It is really important to provide a certainty of evidence rating that reflects the confidence that we have that an estimate of effect is adequate to support a clinical decision or recommendation,” Dahm said. So a GRADE rating of “high” corresponds to “We are very confidence that the true effect lies close to that of the estimate of the effect”. A “very low” rating translates to “We have very limited confidence in the effect estimate: the true effect is likely to be substantially different from the estimate of effect”.
He talked the audience through the GRADE summary of findings table for Cochrane review conducted by urologist Jae Hung Jung (Yonsei University Wonju College of Medicine, Wonju, South Korea) and colleagues and published in 2020, which set out to assess the effects of PAE compared to other procedures for treatment of LUTS in men with BPH. Using an updated version from March 2021, Dahm recounted how the GRADE interpretation of the change in IPSS and quality of life scores following PAE is that there is “little or no difference for these outcomes short-term compared to TURP”. In addition, he said that “we are very uncertain” about PAE having a lower major adverse event rate than TURP. Lastly, he noted that the “greatest certainty” the GRADE reviewers had was regarding retreatment rates in the short-term, which they believed were “probably increased” after PAE.
Quality of evidence for PAE: The IR perspective
Salem offered an interventional radiologist’s perspective, which served as a riposte to Dahm’s previous talk, and detailed the strength of evidence for PAE’s safe and efficacy. While he said he understood the initial scepticism about the success of embolizing the prostate gland, he noted that there have been technical improvements in the procedure since its inception. Furthermore, while attempts at “gold standard” PAE versus TURP trials had failed in the USA, more recent propensity-matched, prospective comparisons of the two procedures and randomised trials of TURP versus sham a procedure are positive indicators that PAE has a positive future.
“More importantly, to Philipp [Dahm]’s point,” Salem commented, “there is a growing patient interest in alternate therapies.”
Following a review of the evidence for PAE, Salem concluded: “In my opinion, no one can say PAE does not work. It does in my opinion satisfy all criteria for a reasonable treatment, and it should be an option presented to patients. At minimum, it should have a limited recommendation for large glands [prostate volumes >80cc], where effectively all of the MISTs [minimally invasive surgical therapies] are ineffective, by the AUA guidelines.
“The AUA guidelines are important, but they are not the final word. Respectfully, no one has a monopoly on the management and the clinical development of managing patients with BPH-LUTS. It should be a team effort. As Philipp said, Level 1 evidence is not the only method of generating high-level, relevant data. Good Phase II data can do that as well—there are ethical and technical challenges with RCTs, as Mark [Little] spoke about.
“Unfortunately, we have been slowed down by—in my opinion—the emotional and polarising reaction by KOLs [key opinion leaders] to evolving PAE data. It is my observation that there is a perceived inconsistency in the manner PAE data are interpreted compared with that [for] MISTs. I think we need to work together, and PAE needs to be offered to the right patient. We need a collaboration between IR and urology, and this collaboration must evolve, not devolve, in a multidisciplinary manner that will benefit patients.”
He ended with a specific request of the attending urologists: “At the end of the day, patients are not satisfied with TURP and MISTs as the only options; they are demanding something else. What I would ask is, given this, what is the pathway for recognition of PAE, at least in a limited scope, [in the AUA guidelines]? If the response is a clinical trial, I would like to know which clinical trial explicitly.”
Offering one urologist’s perspective (with particular emphasis afforded to the “one”), John Kellogg Parsons (Moores UC San Diego Cancer Center, San Diego, USA) took to the virtual podium next. Despite being chair of the AUA BPH guidelines panel, he noted that he was not speaking on behalf of the AUA in any capacity.
He suggested some potential ways forward for interventional radiologists and urologists: “[Look for] other study populations and indications. I think LUTS is unlikely to gain significant traction within the urological community as an indication for performing PAE, so I would encourage you to look for other indications. Haematuria is what I hear constantly as a very compelling indication to investigate, but there are no clinical trials to investigate this. Neoadjuvant therapy, I have heard that hypothesised, I think that is a reasonable avenue to explore; urinary retention and very large prostate, I think that is very reasonable to explore. Always longer term data, and absolutely more multidisciplinary collaboration and coordination.
Addressing his fellow panellists, he said: “I think it is important for this group to know that this field is always rapidly evolving. There is an enormous amount of capital in the private sector in biotech that is investing in newer technologies for BPH. To my knowledge there are at least eight novel urethral stents that are in late phase clinical trials, all with urologists—they come to us when they want to run BPH clinical trials. I would ask you to ask yourselves—the PAE technology, is it static, or dynamic? What kind of future relevance does it have, knowing that this field is constantly evolving with new devices?”
Closing the session, Abt, a principal investigator and sub-investigator in various clinical trials on the treatment of LUTS/BPO (including on PAE, TURP, HoLEP, Aquabeam, and PVP) and a guideline panel member for the Germany Society of Urology document on benign prostatic syndrome, summarised the structural and methodological, problems of guidelines in a bid to understand the reasons for the discrepancies between the SIR and AUA recommendations.
“There are widespread financial and professional conflicts of interest among the sponsors of guidelines, so the societies,” he said, “and also among the authors. Industry funds a network of lobbyists, researchers, and opinion leaders, which then write our guidelines. ‘Panel stacking’ is another problem: if a novel panellist is nominated, they are probably nominated because they believe in the same school of thought, so that leads us to imbalanced guideline panels.”
He commented that the most important part, in his view, is that guidelines often have “highly biased panel compositions”—drawing a “very provocative” comparison, he asked rhetorically: “Which institution would you ask to get the most reliable data on gun violence in the USA? The National Rifle Association (NRA), Americans Against Gun Violence, or a more independent source?
“The same is true for the guidelines for PAE. On the one hand, we have a group of persons that are highly interested in a broad application of PAE, as they work for a society that of course has to represent the interests of their members [indicating the SIR multisociety consensus position statement on PAE for the treatment of LUTS]. The same is absolutely true for the AUA guideline panel.
BPH treatment is a billion-dollar business, and here we have panels where at least some of the people involved have substantial conflicts of interest. In my opinion, it is just plausible that both societies reach different conclusions.”
Abt also touched on the lack of “proper, independent peer-review” prior to the publication of most guidelines, and the idea that recommendations are often provided “despite the data [that form the basis of this advice] being judged as unreliable”.
He agreed with the Institute of Medicine suggestion of removing individuals with a financial conflict of interest from guideline panels, and to implement a limitation on the involvement of clinicians with a professional conflict of interest. “Content experts should be consulted, but not write the guidelines,” he concluded. “Instead, we should use independent statisticians and methodologists, patient representatives, and general practitioners that are interested in the field, but do not earn their money from it.” Abt advocated for the inclusion of a guideline panel review and a checklist to score guidelines ahead of publication, to minimise bias.