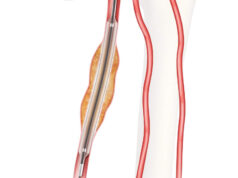
The first 24-month data from the LUTONIX AV investigational device exemption trial were presented at the Charing Cross Symposium in April. These interim data show a sustained effectiveness benefit for the Lutonix drug-coated balloon (BD) and indicate that it leads to an average time to first reintervention that is four months longer than plain balloon angioplasty.
The randomised, prospective, multicentre Lutonix AV trial was designed to assess the safety and effectiveness of the Lutonix 035 drug-coated balloon in the treatment of native dysfunctional arteriovenous fistulae. The patient cohort was a “real-world” group and the study included secondary non-target lesions, de novo/restenotic lesions, and stents in the access circuit outside of the studied lesions. Investigators in the trial randomised 285 patients at 23 clinical sites. After predilatation to specific requirements with a plain angioplasty balloon, patients who had less than 30% residual stenosis were then enrolled and randomised 1:1 to treatment with either a drug-coated balloon or a standard matched compliant percutaneous transluminal angioplasty balloon.
Kate Steiner (consultant interventional radiologist at East and North Hertfordhsire NHS, Stevenage, UK) reported the latest data from the trial. Emphasising the points that would resonate most with patients, she highlighted that patients in the drug-coated balloon arm had, on average, a reintervention at 11 months (318.7 mean days) as compared to patients in the control arm who had a reintervention at seven months (198.4 mean days). “Four months, or 120 reintervention-free days, is significant to the dialysis patient who already spends three days a week on dialysis,” Steiner commented.
The primary efficacy endpoint of LUTONIX AV was target lesion primary patency at 180 days. While the trial did not show a statistically significant benefit for the drug-coated balloon at this time point, further follow-up revealed that the paclitaxel drug had a significant effect on the lesion patency at later time points. The primary safety endpoint was freedom from any serious adverse event(s) involving the arteriovenous access circuit through 30 days and showed that treatment with a drug-coated balloon was non-inferior to treatment with a plain balloon. Follow-up was clinically driven and took place at one, three, six, nine, 12, 18 and 24 month visits.
Steiner maintained that the long-term data suggest a sustained efficacy benefit through the 24 months. “Nowhere in the patency curve do the lines cross through 24 months,” she said, adding that long-term safety remains non-inferior to plain balloon angioplasty. “The Kaplan-Meier patency curves start to separate around the 90 to 100-day mark and what we see now is that they continue to remain separate; there is no time point at which the curves cross or come together. We see a 36.8% improvement out to 550 days and this continues out to a 30% improvement out to 730 days, or 24 months,” she explained.
Results
Results from the study were adjudicated by a core lab, an Independent Clinical Events Committee, and Data Safety Monitoring Board.
The evidence is emerging for the use of drug-coated balloon use in AV access. “When we combine the LUTONIX AV trial, LUTONIX global registry (n=324), and LUTONIX post-approval study (n=213), we will have well over 800 patients going towards addressing the data deficit in dialysis access. I will predict that as we learn more about the pathophysiology of dialysis access stenosis, we will see more innovation in this area,” Steiner stated.