
The Society of Interventional Radiology (SIR) debuted the first-ever virtual reality 360 (VR360) training video showcasing an endovascular transjugular intrahepatic portosystemic shunt (TIPS) procedure in practice, during its Annual Scientific Meeting in March in Los Angeles, USA.
“Virtual reality walks you into a new world. A video like this is a transformative, immersive engagement in a procedure that allows you to adopt, learn and proctor in a completely unprecedented fashion. The pure immersive ability, even in early generations of technology, made it clear to me that this was going to have a major role in medicine,” Ziv J Haskal, a professor with the department of Radiology and Medical Imaging at the University of Virginia Health System in Charlottesville, USA and pioneering editor of the Journal of Vascular and Interventional Radiology (JVIR) told Interventional News.
The one-hour multisegment movie was a special project of SIR’s peer-reviewed journal, JVIR, and was funded by an innovation grant from its publisher Elsevier.
Haskal has recently released a first-of-its-kind, ten-part movie that he has likened to “the Falcon Heavy rocket with the Tesla Roadster on top” that will harness the gifts of virtual reality in endovascular interventions. He has filmed an entire procedure of what is still one of the hardest procedures for people in interventional radiology, TIPS, and segmented it into separate videos. “This procedure is something that I have spent decades trying to perfect. The single most effective way to teach this procedure is in a one-to-one apprenticeship fashion. Those who have not been apprenticed in this fashion do not see the same skill transfer. The totally immersive ability of virtual reality technology will enable such procedures to be taught in another way,” he explained.
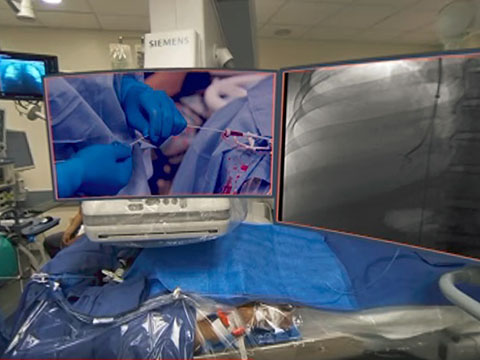
“We have spent a lot of time creating an all-enveloping, in-the-room virtual reality film allowing an operating physician to return to any complex segment they wish for learning, review and perspective. The multicamera shoot and floating high-definition inserts offer viewers every perspective of the case, maximising learning. With the procedure I chose to film, I was teaching on the fly and it will appeal to people on multiple levels who will be able to take something from the training that is beneficial and particular to them. I recently showed it to my mentor, Ernest Ring (Professor Emeritus in the Department of Radiology and Biomedical Imaging at the University of California, San Francisco, USA), who taught how me to do this procedure. He put it on his head and described it as amazing; I could not get it off his head,” Haskal reported.
Hurdles
Commenting on hurdles that might limit further uptake of the technology, Haskal commented that “actually getting people to look at it and put the head set on” is a challenge. “To create a media event for five hundred people and put the box on their head is difficult. It has to be a gradual release, because once people experience the virtual reality video, they are instantly drawn in and excited. I am planning a video to show that it is an easy technology to access; there are multiple platforms and even with an entry level box US$5 they are able to fully access all that virtual reality has to offer.”
The video premiered during the Extreme IR session at SIR 2018 and session attendees received complimentary virtual reality viewers to experience the video on their smart phones.
“Virtual reality is a force multiplier, providing expert training to physicians around the world. I think it will be the future of physician and provider training of new technologies and retention of skills. It will also allow interventionalists the ability to ‘gird their loins’ before going into battle to do a difficult procedure. Virtual reality could also prove to be an invaluable tool to re-train in the use of devices that have not been used for sometime and have become unfamiliar, especially if there is no one available for re-proctoring.
“Virtual reality puts you in that practice environment in a way that is not provided by any other means, which ultimately benefits the patient because you start to absorb information without paying attention to the artifice of a cardboard box on your face,” Haskal maintained.
To see the 10-part movie, navigate your YouTube mobile app to:
https://bit.ly/2KzvWH7
Start a segment, launch the VR view by tapping the Google Cardboard icon, and placing your phone into your VR viewer, be it Cardboard or Samsung Gear. If you have an Oculus or Vive headset, you will see it in the highest resolution and field of view.













