An organised skill development initiative that started in late 2015 offering interventional radiology (IR) training for eight emerging economies has precipitated the development of a global network of trained personnel who can support IR programmes in challenging locations. The initiative has motivated the formation of national IR societies in Nepal, Sri Lanka, Bangladesh and Nigeria, all of which—in addition to Myanmar—now have dedicated IR programmes in their largest hospitals.
The concept and its success is reported in the Journal of Vascular and Interventional Radiology (JVIR) by Sanjiv Sharma and Kartik Ganga (both Department of Cardiovascular Radiology and Endovascular Interventions, All India Institute of Medical Sciences, Ansari Nagar, Delhi, India).
“Integrating IR into clinical practice remains a big challenge in emerging countries in Asia and Africa”, the authors write. “Although IR has changed clinical medicine worldwide, the benefits of these advances have not percolated to the mainstream practice of medicine in these locations. Emerging countries have much to benefit from IR”. With this concept in mind, Sharma and Ganga report how they organised for a group of interested radiologists to travel to their centre and take part in observerships and short-term training courses, typically lasting three months.
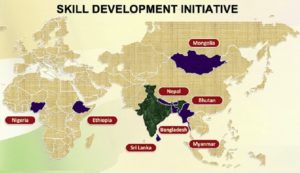
Mongolia, Nepal, Bhutan, Bangladesh, Myanmar, Sri Lanka, Ethiopia and Nigeria were the eight countries that participated in the initiative. Since its inception, 51 specialists from these countries have received observerships in IR procedures. These specialists represent a spectrum of disciplines, including radiologists, technologists and nurses, in order to best help establish a comprehensive IR team in their hospitals, the authors say.
Attendees were provided with logistic and financial support during their training period (up to US$500 per month toward stay and up to US$200 per month for reimbursement of observership), as well as samples of consumables for starting an IR practice and various educational materials. These included textbooks and management protocols published by the Society of Interventional Radiology (SIR) and the Cardiovascular and Interventional Radiological Society of Europe (CIRSE).
A further 15 educational events have also been conducted to international audiences to date, some at the authors’ own institution and some within the participating countries’ borders. “Emphasis was placed on teaching and building standards for the ethical practice of IR”, according to the study authors. There is currently no exit-level examination following training, but Sharma and Ganga state that they intend to introduce one this year. To further objectify the results of the initiative, they are designing a survey to assess the impact of their training scheme on alumni who have returned to their native hospitals and started their own specialty practice.
Trainees establishing their own practice was one of the target outcomes of the initiative. Sharma and Ganga explain that trainees “were encouraged to start an IR practice [on return to their native countries] and were supported in decision making and procedure planning by regular communication via various channels, including telephone, WhatsApp, and e-mail on a regular basis”. CME programmes and workshops in their local institutions reinforced this training, and periodic invitations to conferences held at the All India Institute of Medical Sciences updated this learning.
Another key component of the training initiative was to use web-based platforms as “force multipliers”, allowing for wider participation. Virtual lectures and CME programmes were held for audiences across Asia and Africa, and were in fact transmitted live to up to 56 countries.
Radiology residents at medical colleges in India with poor IR utilisation were offered a short stint at an established IR department to raise awareness of the discipline and to encourage recruitment. This aimed to provide first-hand learning experience to acquire basic IR skills, as well as networking opportunities.
This global network building is key: Sharma and Ganga attribute the success of the programme to the participation of experienced interventional radiologists from India, the USA, China, Germany and the UK. “These individuals act as global ambassadors for IR and play an enormous role in both inspiring and imparting knowledge to the budding specialists as well as act as role models for them”, they say.
Sharma and Ganga have also shared a collaboration with the International Atomic Energy Agency (IAEA) to prepare a document outlining the relevance of IR in clinical medicine and methods of establishing it in emerging countries. An expert group formed under the aegis of the IAEA in 2015 has published a report entitled The Needs of IR in Emerging World Countries. Keeping in mind that IR is variously recognised as a subspecialty of diagnostic radiology or is a distinct clinical specialty, Sharma and Ganga impress upon their readers the importance of establishing IR as its own specialty in Asia and Africa. Their work with the IAEA aims to lay stress on this issue.
Collaborating with national and international centres of excellence and setting up more training centres are among the next objectives, according to Sharma and Ganga. They call for large international IR societies to lend their experience and organisation to help support this cause, concluding: “Problems with availability of IR equipment should be addressed by encouraging and fostering indigenisation and locoregional development of such technologies. Until IR gets incorporated and integrated into regional health care systems and university teaching programmes, the nascent regional IR community needs the support of international IR organisations.
“Our specialty shares natural collegial bonds that should be harnessed to help grow rather than wait for external governmental agencies to leapfrog administrative and financial red tape and sluggishness”.
The possibility of spreading interventional radiology across the globe is also one which excited Vincent Vidal, whose FAIR-Embo concept aims to enable the use of an inexpensive and widely available embolization agent to perform minimally invasive procedures.








