
“There is a general misconception that you cannot do interventional radiology (IR) in a resource limited setting,” says Fabian Laage Gaupp, IR resident at Yale School of Medicine (New Haven, USA), and a member of the Yale Radiology Outreach Program. He is outlining his work alongside colleagues to establish a radiology service at the Muhimbili National Hospital campus in Dar es Salaam, Tanzania, East Africa. “From having done this for almost three years, I can say that this is simply not true,” he says, picking up on the earlier statement.
The initiative has seen more than 50 volunteers travel to Tanzania in teams of up to five for two-week placements to provide hands-on training to radiology residents, nurses and technologists. Funded initially through donations and institutional grants, the project has recently been awarded funding through the Radiological Society of North America (RSNA) Derek Harwood-Nash International Education Scholar Grant scheme, which Laage Gaupp says will help to continue the initiative into the immediate future.
The project has grown out of work begun by Yale’s director of neuroradiology MRI and assistant professor of neuroradiology, Frank Minja, who initially sought to implement a Picture Archiving and Communication System (PACS) at the Muhimbili Orthopaedic Institute in Dar Es Salaam in 2014. Since then, Minja has made regular trips to Tanzania—the country of his birth—to support physician training in the country. Minja crossed paths with Laage Gaupp, who joined Yale as a radiology resident in 2016, and, hungry for outreach opportunities within the IR field himself, joined Minja on a trip to Dar es Salaam in 2017.
“In Africa you have around 1.3 billion people currently, and there are really only two countries where IR is established—South Africa and Egypt,” says Laage Gaupp, discussing the demand for IR services across the continent. Tanzania has a population of over 50 million, including over four million in Dar es Salaam, the country’s most populous city and the focal point of the outreach programme. During his first trip to the country, Laage Gaupp armed himself with an Interventional Radiology Readiness Assessment tool to establish the scope for setting up an IR service within the country. In terms of the availability of imaging equipment to support IR work, he found that this could be feasible, but the disposable equipment needed was lacking. Undeterred, he set about designing a training scheme that could bring IR into the country.
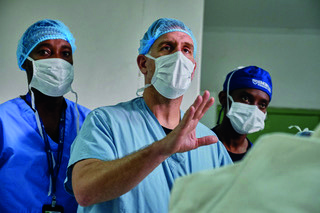
“We have followed the same training model that we do in the USA, doing three years of diagnostic radiology, followed by two years of an IR residency. In Tanzania they already have the three years of diagnostic radiology residency, so we essentially just have to add two years of interventional radiology.”
To date, six residents have enrolled over two year groups, with the first group of three residents set to graduate in September 2021. They are undertaking a combination of on-the-job training and lectures delivered by the visiting groups from institutions across the USA and Europe. Visiting groups, who visit for two weeks at a time, comprise at least one physician, nurse, and technologist, reflecting the fact that IR is, in Laage Gaupp’s words, “a team sport”. Groups may also be augmented by medical students and radiology residents. The ultimate aim of the programme is the establishment of a self-sustaining IR residency programme at Muhimbili, with Tanzanian IR faculty training Tanzanian residents. “Our focus has always been on getting them to be able to work independently quickly and we are already starting to see the outcomes of that,” Laage Gaupp comments. “They are already doing a lot of procedures independently, so now on a daily basis they do CT and ultrasound guided core needle biopsies, they do nephrostomy placements, and they do biliary drain placements, which is really considered a technically challenging procedure in many cases. There is no trained IR attending in Tanzania, but they are able to provide these really life-saving procedures, and have great success.”
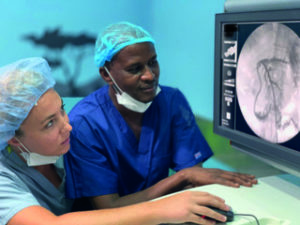
The course has been designed to begin with teaching residents more basic procedures: “those that are more necessary”, Laage Gaupp says, such as core needle biopsies. “That might not be considered a life-saving procedure, but it is extremely necessary, because until then people were only doing fine needle aspiration, which has a much lower diagnostic yield.
“We felt that is something that would have a really significant impact on patient care because it is going to help you diagnose and help to guide the treatment. At the same time, it is a simple procedure where you can learn [to use] image guidance and you have a lower chance for complications.” Other procedures, including abscess drainage and nephrostomy and biliary drainage, have been prioritised, due to the potential impact these could have on morbidity and mortality compared to surgery. “Just by making those procedures available, that is the highest return in terms of patient outcomes that you can have. Even with those really basic procedures, you are going from a patient dying, to that patient surviving,” he emphasises.
Discussing some of the differences in running an IR service in East Africa, compared to the USA, Laage Gaupp comments that there is a significant difference in the “disease spectrum” of patients using healthcare services in Tanzania, with a high prevalence of parasitic infections, for example, as well as in the stage at which patients present in-hospital for treatment. “People present a lot later in general [in Tanzania],” Laage Gaupp remarks. “In the USA in particular, when people have the slightest headache or stomach ache, they usually go and see a doctor. In Tanzania, the coverage is different. For someone from a rural area to actually present to the national hospital in Dar es Salam takes months or sometimes years. Until they get to the national hospital, those are really the sickest of the sick, people show up with huge tumours, with roaring infections, with anything under the sun.”
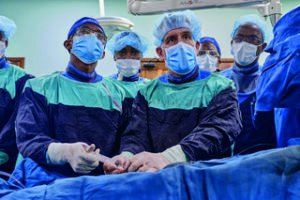
Another aspect he notes as being specific to Africa is a higher percentage of paediatric patients. “While paediatric interventional radiology in the USA is considered a bit of a fringe subset of IR, in sub Saharan Africa, paediatric interventional radiology will play a pretty big role because there are so many paediatric patients,” he notes. He also points to a large prevalence of uterine fibroids, which is particularly notable in black women compared to in predominantly white or Asian populations, adding that the introduction of uterine fibroid embolization (UFE) has the potential to have a huge benefit in throughout the region.
“If you look at UFE in particular, and you compare it with hysterectomy, one of the most common procedures worldwide, complication rates in sub Saharan Africa are on average higher than in Europe or the USA,” Laage Gaupp comments. “Now with UFE, the procedural risk is much lower, and second of all you do not need general anaesthesia, so you are taking that risk out. It is such a common problem, even if you said IR was limited only to UFE, that alone would justify bringing IR to sub Saharan Africa.”
The outbreak of COVID-19 has meant that outreach trips have been cancelled until it is safe to travel again. Laage Gaupp hopes that this will be before the end of 2020, but faculty have been able to offer online education through video conferencing. “If there is a positive thing that has come from COVID-19, it is the access to online teaching,” he comments, but notes that there is “no substitute” for hands-on teaching, particularly within IR.








