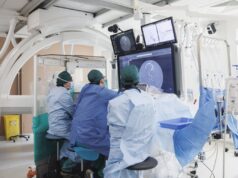
Addressing the importance of radiation protection for the modern interventionist, Kevin Mani writes about the need for knowledge and training in radiation protection for vascular surgeons and interventionalists, and radiation protection as an integrated part of training.
The majority of vascular surgical procedures are today performed with endovascular techniques. The massive increase in the number of endovascular procedures, as well as the increasing complexity of these procedures, necessitates that specific attention is paid to the risks associated with radiation exposure in relation to endovascular surgery.
The repetitive exposure of modern interventionists to high radiation doses is of major concern. Several pioneers in the vascular surgeon interventionalist community have paid a high price for the developments made in endovascular surgery during their time in practice due to excessive radiation exposure, with development of radiation induced cataract as well as neoplasms. Although knowledge regarding the true risks with occupational radiation exposure is still scarce, recent studies indicate that measurable DNA damage among operators occurs already after a simple EVAR procedure.1 Additionally, there are indications of higher prevalence of left-sided brain tumours among physicians with occupational exposure to interventional radiation.
Strategies
Measures to reduce occupational radiation exposure during endovascular procedures are twofold: 1) reducing the radiation dose, and 2) applying adequate protection to reduce scatter radiation. Reduction of radiation dose adheres to the “as low as reasonably achievable” (ALARA) principle, which mandates medical use of X-rays to be limited to the lowest possible dose. In endovascular surgery, this is based on cautious and meticulous X-ray technique. Measures to reduce radiation dose include application of adjusted low dose programmes with minimum pulse frequency and radiation energy which are tailored for the type of endovascular procedure being performed. Such targeted fluoroscopy and angiography algorithms can be developed together with interested hospital physicists in collaboration with the major providers of imaging equipment. Adequate use of beam collimation, digital image magnification, 2D-3D fusion and image overlay are other methods proven to reduce the exposed field and required radiation.2 Reduction of the radiation dose has important benefits both for the patient as well as for the personnel. Real-time dosimeters used by the operating room personnel offers a possibility for direct feedback regarding radiation exposure, in order to increase awareness and modify behaviour.
Adequate protection
In addition to the reduction of radiation dose, use of adequate protection is key to reduce occupational radiation exposure during endovascular procedures. Radiation protection measures can be classified into two groups: 1) radiation shields placed close to the patient, reducing scatter radiation from the patient in general, and 2) radiation protection placed close to or worn by the personnel. Ceiling suspended shields, table mounted shields and disposable radiation-absorbing surgical drapes such as RadPad all encompass radiation protection close to the patient. A properly used combination of these shields can successfully reduce scatter radiation with >80%. The functionality of shields placed close to the patient is however highly dependent on adequate positioning of the shields. Challenges to correct use of these protective shields during complex endovascular surgery include collision of ceiling mounted shields and operating light or flat panel detector, lack of adequate shielding during lateral projection fluoroscopy/angiography, and lack of protection on the patient’s left side during interventions performed, e.g. from left brachial or axillary access.
Basic protective shielding for personnel includes the use of a lead apron and thyroid shield, complemented with protective glasses. Considering that the eye lens is the most radiation sensitive organ, eye protection should be a key element for all endovascular operators. Interestingly, experimental data suggest that the dose reduction effect of protective eye glasses varies significantly between different models, with the majority of the commercially available eye glasses offering a moderate 10–15% dose reduction at left eye. The dose reduction effect is highly dependent on the size of the gutters between the protective glass and the skin. Therefore, protective glasses should be tailored to each operator, with close fit and large protection area.
Additional risk and options
Even with standard lead apron and eye glasses, significant body areas including the arms, shins and head remain unprotected to scatter radiation, which may pose a risk especially for the primary operator closest to the source of scatter radiation. The landmark study by El Sayed et al showing radiation-induced DNA damage in EVAR operators could also verify that DNA damage can be reduced by additional use of radiation-protective shin guards. Optimal radiation protection would include protection for all exposed body areas. However, additional shielding may also be cumbersome and result in excessive weight, potentially with negative effects such as back pain and lumbar hernias. The suspended lead suit radiation protection system (ZeroGravity radiation suit) is an attempt to offer near to full radiation shielding without additional weight on the operator’s body. The system is based on a thick lead suit with a curved lead-acrylic head shield that is suspended either from a ceiling mounted monorail, repositionable floor unit, or a hinged swing arm. The ZeroGravity system offers excellent radiation protection for the primary operator, with significant reduction of the radiation exposure to the head, upper arms, and legs, in addition to what is today achieved with standard lead apron, Figure 1. In a recent assessment of the system in neuro-endovascular intervention, the suspended lead suit resulted in an additional 75% reduction in the operator-received total dose compared to standard protection including lead apron, glasses, ceiling and table-mounted shields.3 There is, however, still potential for further development. In our experience, the weight of the floor mounted ZeroGravity system may hinder repositioning possibilities. Additionally, a relatively high cost of acquiring the system may limit its use to high-volume endovascular centres.
Awareness

The increasing number of endovascular procedures in the field of vascular surgery is likely to continue in the future. This results in a need for knowledge and training in radiation protection for modern interventionists, and radiation protection is increasingly an integrated part of vascular surgical training. Although basic protection is achieved with adherence to the ALARA principle and the use of regular protective shields, the risk of repetitive occupational radiation exposure for interventionists remains a concern. Further innovation in endovascular surgery and radiation protection will play an important role in achieving the ultimate goal of zero radiation exposure during these procedures.
Kevin Mani is associate professor of vascular surgery at the Department of Surgical Sciences, Uppsala University, Uppsala, Sweden.
References
1. El-Sayed T, Patel AS, Cho JS, Kelly JA, Ludwinski FE, Saha P, Lyons OT, Smith A, Modarai B, Guy’s and St Thomas’ Cardiovascular Research C. Radiation-Induced DNA Damage in Operators Performing Endovascular Aortic Repair. Circulation. 2017;136:2406-2416.
2. Hertault A, Maurel B, Midulla M, Bordier C, Desponds L, Saeed Kilani M, Sobocinski J and Haulon S. Editor’s Choice – Minimizing Radiation Exposure During Endovascular Procedures: Basic Knowledge, Literature Review, and Reporting Standards. Eur J Vasc Endovasc Surg. 2015;50:21-36.
3. Haussen DC, Van Der Bom IM and Nogueira RG. A prospective case control comparison of the ZeroGravity system versus a standard lead apron as radiation protection strategy in neuroendovascular procedures. Journal of neurointerventional surgery. 2016;8:1052-5.