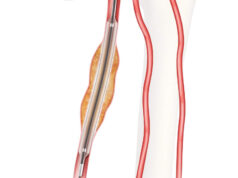
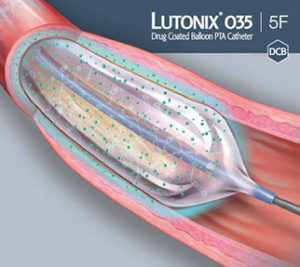
 The 24-month results of the worldwide experience with Lutonix 035 drug-coated balloon (CR Bard/Beckton Dickenson) were published online in August in JACC: Cardiovascular Interventions. Data revealed that patients with femoropopliteal lesions who were treated with the drug-coated balloon experienced symptom improvement and that low reintervention rates were observed at 24 months, even in patients with difficult-to-treat lesions.
The 24-month results of the worldwide experience with Lutonix 035 drug-coated balloon (CR Bard/Beckton Dickenson) were published online in August in JACC: Cardiovascular Interventions. Data revealed that patients with femoropopliteal lesions who were treated with the drug-coated balloon experienced symptom improvement and that low reintervention rates were observed at 24 months, even in patients with difficult-to-treat lesions.
Marcus Thieme, Sonneberg, Germany and colleagues report that outcomes from the registry at two-years confirm Lutonix is a “safe and effective long-term treatment option in real-world patients with peripheral arterial disease with superficial femoral artery lesions.” These outcomes were also achieved in patients with long lesions and in-stent restenosis.
As reported in JACC: Cardiovascular Interventions, the Global SFA registry is a multicentre, prospective study that enrolled 691 patients in 38 centres from 10 countries. These patients were treated with the Lutonix 035 DCB in femoropopliteal lesions. The registry set out to assess safety, clinical benefit, and outcomes of the Lutonix 035 drug-coated balloon in a heterogeneous, real-world patient population at 12 and 24 months.
Freedom from a composite of target vessel restenosis, major index limb amputation, and device- or procedure-related death at 30 days was defined as the primary endpoint. “The primary effectiveness endpoint was freedom from target lesion restenosis at 12 months. Secondary endpoints were acute device and procedural success and clinically assessed primary patency,” the authors write.
Results
The registry results showed a 99.4% freedom at 30 days from the composite safety endpoint. There was 89.3% freedom from target lesion restenosis in the overall population at 24 months. In long lesions up to 50cm, the freedom from target lesion restenosis was 88.2%; in patients with in-stent restenosis this figure was 84.6%. The clinically assessed primary patency was 75.6% and more than 76% of patients showed improvement of at least one Rutherford category.
Editorial comment
In an accompanying editorial comment in the journal, Ivan P Casserly, Dublin, Ireland, writes: “Most endovascular specialists are inherently attracted to the use of drug-coated balloon angioplasty as the primary strategy for revascularisation of the femoropopliteal segment. This is driven by several considerations. Primarily, the greatest concern is to avoid the spectre of in-stent restenosis, for which there is no good therapy. If a durable result can be achieved with drug-coated balloon angioplasty, even if it has lower primary patency rates compared with drug-eluting stent, then this option would generally be favoured. In addition, angioplasty is ‘very straightforward’, resulting in a reasonably predicatable outcome across a broad range of operators.”