This advertorial is sponsored by Inari Medical.
A recent Inari Medical roundtable webinar examined how to build a venous practice effectively—three experts from different specialties discussed the importance of forming and maintaining internal and external networks; what to consider when building a deep vein thrombosis (DVT) pathway; and how to choose the right treatment for each DVT patient. The webinar is part of the first edition of the ClotWarrior Academy DVT Webinar Programme set up by Inari Medical to initiate further education and conversation around the effective management and treatment of the full range of DVT chronicity.



Stephen Black, vascular surgeon at Guy’s and St Thomas’ NHS Foundation Trust (London, UK) began proceedings, focusing on “the power of the multidisciplinary team”. Black also pinpointed how crucial it is to know the data and the literature relating to venous work, as well as to spend time with “people who have done it” before and “utilise their skill”—namely, those with established practices. In terms of data, there are more to come, Black added. “We have launched DEFIANCE, a randomised controlled trial (RCT) evaluating its clinical outcome in DVT treatment. Its goal is to demonstrate that mechanical thrombectomy is superior to anticoagulation alone. Other RCTs in the DVT space have all focused on catheter-delivered lytics and we know that the downside of lytics is bleeding, which was a significant outcome of the ATTRACT study. Trying to find something that avoids lytics is going to be really useful for this therapy.”
In terms of building the team, Black made the point that venous patients can be “more needy than their arterial [counterparts]”, and so lots of staff from different departments need to be involved in their care, including in theatre, interventional radiology (IR), haematology, ultrasonic angiology, and research. Black emphasised that even the intervention itself can be multidisciplinary depending on circumstances, with “another member of the team finishing it off”. He then touched on the protective, supportive aspect of working as a team—“if something goes wrong, […] and it will, you are very vulnerable if you are by yourself […]”, whereas as part of a team, this is guarded against.
Next, Black addressed how introducing pathways into the hospital is key “because you cannot be there all the time” to oversee every patient’s referral and care. These pathways enable smooth follow-up and decision-making around “who to treat and who not to treat”. Having an eye for detail is also important, he continued, stating that “it is not good enough to [just] hope for the best”.
After the procedure, Black advocates for duplex follow-up, then reflecting on the outcome, and repeating this after every procedure, having considered the success of factors such as “stent choice and placement, errors, and IVUS”. Moreover, he suggested that “most errors of a technical nature are the fault of the user, not the product”. Returning each time to consider outcomes will ensure that they keep getting “better and better”, Black averred.
Michael Piorkowski, interventional angiologist and cardiologist at CCB Frankfurt (Frankfurt, Germany) was next to speak, first outlining how the interventional DVT programme at his centre started. He described his hospital’s large cardiovascular outpatient service and how “every day, there are up to ten patients referred from general practice with suspected DVT”. The programme has office hours of 8am to 6pm Monday to Friday, with various lab testing capabilities as well as those for other types of imaging, including several vascular ultrasound machines and computed tomography (CT) and magnetic resonance imaging (MRI) with cardiovascular-specialised radiologists.
“When I started here in 2014, the majority of patients, even those with iliofemoral DVT, were treated with compression stockings and oral anticoagulation,” Piorkowski relayed, going on to say that when he first treated acute DVT in 2012, he used a rotational thrombectomy device. He then switched to a pharmacomechanical aspiration device but “most patients still also had some form of lysis”. This limited the indication, Piorkowski went on, adding that the research at the time was also not really venturing beyond chronic venous disease.
Nowadays, he noted that they still see patients who underwent DVT treatment 10 or 15 years ago—“there is a high patient loyalty”. They have started to treat chronic venous occlusions, especially in middle-aged women who experienced an iliofemoral DVT in their twenties or following childbirth. “There is a growing recognition of the need for a treatment with high thrombus removal and without lytics,” Piorkowski then affirmed. “We were one of the first centres outside of the US to introduce the ClotTriever system and in my opinion this is the most efficient way to remove acute and chronic clots. I faced the problems of patients developing PTS over the long term, including problems with varicose veins, leg ulceration, constant heaviness and swelling of the legs. By removing all of the clot, in the acute phase, we can prevent all of this.
Gerd Grözinger, interventional radiologist at the University of Tübingen (Tübingen, Germany) followed Piorkowski, sharing his experience of how he takes on DVT referrals. Firstly, he outlined an example of a case he has seen—a 30-year-old woman with five-day-old leg pain, who had never had thrombosis before nor had a family history of it. She took the contraceptive pill and was a smoker, Grözinger shared. She received an ultrasound, which confirmed the DVT, and she was then referred to Tübingen. This led Grözinger to make the point that networks of hospitals including specialist centres are crucial in providing adequate care for DVT, so that hospitals in rural areas that may not have the required expertise can work with bigger, more specialised hospitals to refer their patients over if necessary.
“The team is very important,” he continued, expanding on this to describe his hospital’s vascular centre, which has all the specialties combined, including vascular surgery, cardiology, angiology, IR and dermatology. There are two vascular board team meetings each week, at which DVT patients are discussed, and a 24/7 service for vascular emergencies, Grözinger detailed. Different external specialists refer DVT patients to the vascular centre, including internal medicine and emergency departments, and primary care physicians.
Grözinger then highlighted a “holistic approach” as key, which, at his centre, means they have a linked pulmonary embolism (PE) team, and often see patients who are being seen, for example, by oncology for metastatic lymph nodes in the pelvis, which has gone on to cause compression disease and subsequently DVT. Standardised treatment pathways for DVT and PE are necessary, he stipulated. Grözinger shared that, at his hospital, their DVT pathway is mostly based on the European Society of Cardiology guidelines. “All patients with a proximal DVT have cross-sectional imaging with MRI, as it is the only modality that can assess the real age of the thrombus”.
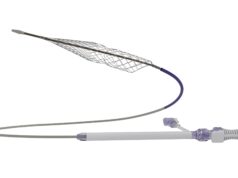
“I think we all have to consider that DVT is not a life-threatening condition,” Grözinger then mused, reflecting on how the bleeding risk with treatments including catheter-directed thrombolysis (CDT) may not be worth it. Therefore, there is “a need for a mechanical thrombectomy system without CDT”—ClotTriever (Inari Medical) is an answer to this need, he put forward. “The system is a mechanical thrombectomy system designed to remove large thrombi from large vessels in a single session, without the need for thrombolytic drugs or consequent intensive care stay. The patient I mentioned earlier, who was referred to us, was also treated with ClotTriever system. She had a complete occlusion and the clot which we removed during the intervention was organised thrombus. This is what we experience in a number of patients—they develop chronic DVT and thrombolysis would not work in those cases.”
Grözinger’s last word was on increasing the visibility of this “undertreated disease”, which he believes can be achieved with “satisfied patients with quick improvement of symptoms”. He would also advise good communication about cases with the referring centre beforehand, and offering lectures and educational material to these referring physicians to “raise awareness”.
To learn more about the lytic-free mechanical thrombectomy ClotTriever and FlowTriever systems, join Inari’s symposium at CIRSE 2023 on Sunday 10 September at 1pm (Auditorium 15).