Speaking at the 2019 annual meeting of the Cardiovascular and Interventional Radiology Society of Europe (CIRSE; 7–10 September, Barcelona, Spain), Vincent Vidal (Marseille, France) describes the Fair-Embo technique, detailing how to obtain the inexpensive embolic agents, the technical efficacy of the procedure, and his ambitions for the project’s future.
An initial preclinical study in a porcine model tested the feasibility and safety of arterial embolization with absorbable and nonabsorbable suture fragments. The investigators reported a technical success, demonstrating the proof of concept of the feasibility and safety of the so-called “FAIREmbo” procedure. Demonstrating the in vivo feasibility of the procedure led Vidal and colleagues to propose what they termed the “FAIR-Embo technique”. Writing in Cardiovascular and Interventional Radiology (CVIR) earlier this year, they concluded: “Embolization by absorbable and non-absorbable suture is a feasible and effective treatment, which opens up the possibility of global use of this inexpensive and widely available embolization agent”.
At present, Vidal is working with the French Society of Radiology (FSR) to send out a survey to countries with emerging economies—“potential Fair-Embo recipients”, in his words—to map interventional radiology services around the world. The survey will be sent to more than 3,000 email addresses across Africa, South America, Asia, the Middle East and eastern Europe. The survey asks basic questions about access to interventional radiology services, such as:
- Do you have access to interventional radiology in your hospital/ town/ state/ country?
- If yes, which kind of procedures are regularly performed: angioplasty? Embolization? Drainage?
- How many interventional radiologists are working in your hospital/ town/ state/country?
- Do you have a contact with a local or national interventional radiology organisation or scientific society?
- Do you have any difficulty with obtaining implantable medical devices?
Although the survey results are yet to be received, Vidal speaks to Interventional News about his expectations. He tells this paper that he anticipates the results “mapping the places where interventional radiology is possible”, as the answers will delineate where in the world trained physicians are working, the availability of imaging hardware such as X-ray machines, and where access to implantable medical devices is an issue. “The final goal”, he says, “is to target the places where FAIR-Embo will be helpful, and also where the existence of an educational programme will be useful as a first point of action”.
With this in mind, the future steps of the Fair-Embo project that Vidal envisions centre around creating a global community of interventional radiologists. Initially, he plans to create a foundation with the capacity to fund a FAIR-Embo clinical programme in developing nations. Outlining this idea to Interventional News, Vidal enumerates the features of this potential future foundation: “We will get help from a proctor if necessary to set it up. I foresee the foundation as one which can offer tips and tricks to interventional radiologists working in low resource settings, which will help provide any necessary materials, and which can help elaborate an existing clinical research programme.”
Further to the development of a FAIR-Embo foundation, Vidal would like to link this with “all the interventional radiology organisations around the world”. Ambitious in his aims for the project, Vidal says that he would like to collect data from the FAIR-Embo community (such as the number and outcomes of embolizations performed) “in order to give feedback to international healthcare organisations such as the International Atomic Energy Agency (IAEA) and the World Health Organisation (WHO)”.
By taking these steps, Vidal hopes to create “a virtuous cycle”. He imagines it working thus: FAIR-Embo will help to develop embolization practices in low resource settings; data collected from these procedures will help to obtain funding from international organisations; this funding will help interventional radiology research in the form of the development of clinical programmes in emerging countries.

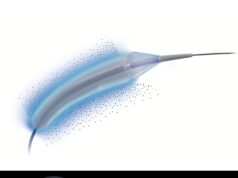
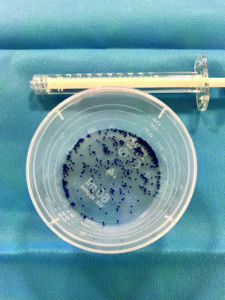
At CIRSE, Vidal presented a new study demonstrating how to obtain non-spherical particles with suture material. Using scissors, he advises interventional radiologists to cut sutures into small fragments between 700 and 1,100 microns long. So called “FAIR particles” (Figure 1) are then injected via a catheter to the target site, and their technical success is demonstrated through post-embolization imaging (Figure 2).
Afshin Gangi (Strasbourg, France), CIRSE vice-president, is enthusiastic about FAIR-Embo, commenting: “Even if this concept is not adapted for all cases, if this material becomes clinically available [as an embolic agent], it will be a game changer for developing and even for industrial countries.”
Detailing why he thinks this, Gangi says to Interventional News: “Traumatic, post-partum or post-surgical bleeding is a major cause of mortality. Until the late 1970s, operative management was considered the only legitimate course for blunt and penetrating abdominal and extremity vascular injuries. Interventional techniques first popularised in the early 1970s now offer a wide range of solutions, principally using transcatheter arterial embolization. Various embolic agents (for example, coils or gelfoam) and particles may be used to stop or control bleeding. All these agents used individually or in combination can save lives by stopping life-threatening bleeding.
“An embolization performed by a well-trained interventional radiologist is essential in all centres dealing with bleeding—trauma centres, maternity wards, surgical units where high blood loss is common, to name a few. In developing countries, training interventional radiologists to safely perform embolization is key. However, regardless of IR training or the presence of an angiosuite with high resolution C-arm fluoroscopy capabilities, availability of the embolic agent is an issue. The idea of having an efficient embolic agent which is available anywhere and is cost-effective is very attractive.
“The idea underpinning ‘the FAIR-Embo concept’, which demonstrates the feasibility and efficacy of using non-absorbable and absorbable sutures, is about making a cheap embolic agent available everywhere. In addition to this availability, the benefits of this material are that it is inexpensive, can be temporary or permanent, that it leads to mechanical obstruction, and that suture fragments are easy to work with.”