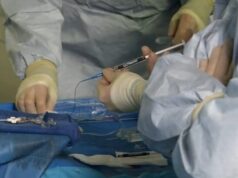
As part of the ‘Trauma and Emergencies’ session at this year’s European Conference on Embolotherapy (22–25 June, Nice, France), conference deputy chairman Otto van Delden (Amsterdam University Medical Centers, Amsterdam, The Netherlands) presented blunt abdominal trauma cases to delegates “to underscore the teaching points” that these types of clinical scenarios offer. In the course of his presentation, he addressed key questions an interventional radiologist (IR) may have regarding the treatment of blunt abdominal trauma, including “which embolic agent and technique [you should] choose for the most frequently encountered injuries.”
A noteworthy feature of this session overall was audience interaction; with each case presented, the speaker posed the question of whether to embolize and, if so, which agent to use, to the floor, before commenting on how closely the consensus from the room aligned with their preferences and choice in the real-life scenario about which they were speaking. Van Delden’s presentation gave him opportunity to convey his feeling that “blush” on a computed tomography (CT) image—indicative of vascular injury—is not a solely sufficient reason for embolizing, but that when it does not “resolve itself”, and the IR has also taken into account “age, coagulopathy and fragility”, it can be a good approach.
In both the cases van Delden put to the audience, opinion was split down the middle on whether or not to embolize, highlighting the multifaceted decision-making involved in intervening in these trauma situations. Van Delden summarised for the audience that, if they themselves are faced with the question of whether or not to embolize, the factors to consider are the extent of organ injury, haemoperitoneum, and vascular lesions, which can be seen on CT. Expanding on this, van Delden listed some of the vascular lesions, in the presence of which, embolization may be indicated: active extravasation outside or within the organ, and false aneurysm. If high-grade organ injury or enlarging haemoperitoneum show on a CT scan, then these are “predictors” of an embolization, van Delden also noted.
Coils were the most popular means of embolization among audience members for the cases van Delden presented, with 71% of the vote for the splenic injury case, which was one of those detailed by the presenter. Although coils may be a favoured choice, “you need to choose the size carefully,” van Delden cautioned, as it is essential not to occlude too much vessel, nor to have the coil move within it.
Then addressing the question of proximal or distal embolization, van Delden acknowledged that “there is no consensus” on which is best, and that it can be down to IRs’ preferences as individuals and “multiple different variables.”
“Tortuosity of vessels” and “time pressure” also come into embolization-related decisions, the presenter added, reinforcing his earlier point that embolization for trauma can divide opinion and resist consensus. “Although coils are the mainstay for treating liver injury,” a little over the majority of voting delegates would have chosen a gelfoam agent in the instance shown on screen by Van Delden, who conceded that depending on coagulopathy, a non-coil embolization may be more suitable.