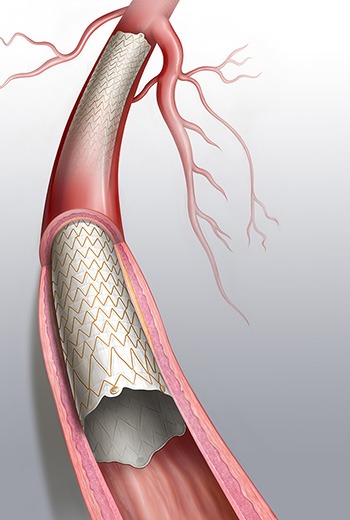
The Covera vascular covered stent (BD) has a superior six-month primary patency rate than standard balloon angioplasty, with an equivalent safety at 30 days, when used in the treatment of stenotic lesions in arteriovenous (AV) fistula patients. Data from AVeNEW, the first level-one clinical trial on the use of a covered stent to treat these patients, were reported at the Cardiovascular and Interventional Radiological Society of Europe (CIRSE; 22–25 September 2018, Lisbon, Porugal).
Principal investigator Bart Dolmatch (Department of Radiology, Palo Alto Medical Foundation, Mountain View, USA) told delegates: “The primary endpoint was six-month target lesion primary patency, and in the covered stent group the primary patency was 78.7%, whereas in the angioplasty group it was 47.9%; that is greater than 30% difference at six months, with a P value that was highly significant at <0.001.”
The primary safety endpoint was measured by freedom from an event resulting in intervention, hospitalisation, or death at 30 days. The study found that use of the vascular covered stent was non-inferior to percutaneous transluminal angioplasty (PTA) alone.
Dolmatch said: “You can see a comparable safety profile for both the covered stent group and the angioplasty group, with a high significance for showing non-inferiority of the Covera stent graft compared to angioplasty.”
The prospective, international multicentre study randomised 280 patients (1:1) to receive either balloon angioplasty or angioplasty plus the Covera stent graft for the treatment of stenotic lesions in the venous outflow of upper extremity AV access circuits in patients dialysing with an autogenous fistula. The Covera vascular covered stent is a polytetrafluoroethylene- (ePTFE) covered selfexpanding stent. Patients were treated at 24 centres in the USA, Europe, Australia, and New Zealand, and exhibited greater than 50% stenosis in the venous outflow of the AV access circuit, with clinical or haemodynamic evidence of fistula dysfunction.
Dolmatch explained: “The study included the typical sort of dialysis patients we see across the globe, with a mean age of about 62 to 63 years, slightly more weighted towards males than females, and about 30% of patients had a BMI [body mass index] that was… in the obese or heavy range. The patients had typically brachial cephalic or brachial basilic fistulae.”
Secondary measures included access circuit primary patency and the number of reinterventions needed to maintain patency. The number of target lesion reinterventions for the covered stent group was 0.3 for the six-month period, compared to 0.8 for the angioplasty group. Acute technical and procedural success rates were also high in the stent group, at 100% and 98.6%. “Overall,” said Dolmatch, “the procedure was extremely successful, with a very low complication rate.”
He added: “All of the stent graft sub-analyses showed superior outcomes compared to balloon angioplasty—for instance, the use of treatment in the cephalic vein arch, with much better outcomes with the stent graft group compared to angioplasty.” The vascular covered stent had a success rate of 78.7% in the cephalic vein arch versus 38.3% for PTA alone, a difference of 37%. Target lesion primary patency was maintained in 86% of de novo lesions and 77.7% of restenosed lesions in the stent group, compared to 65.6% and 40%, respectively, for angioplasty alone.
The most commonly used diameters of stent graft used in the study were nine and 10mm, and stent graft lengths were typically between 40 and 60 diameters.
Follow up in the AveNEW trial is ongoing for two years, and Dolmatch expressed his optimism about future results. “The divergence [in primary patency] is really starting at about 60 days and continuing on to 180 days. This is six-month data. We are looking forward to seeing 12-month, 18-, and 24-month data showing the superiority of stent graft treatment of the stenoses in fistulae, compared to angioplasty.”










