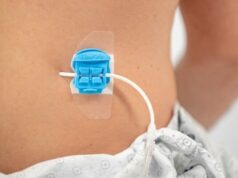
For most patients receiving systemic anticancer treatment (SACT), totally implanted ports (PORTs) are more effective and safer than both Hickman-type tunnelled catheters (Hickman) and peripherally inserted central catheters (PICCs). The CAVA trial’s results, just published online in The Lancet, recommend reshaping current guidelines and practice, so that most patients requiring chemotherapy for solid tumours receive a PORT within the UK National Health Service, foreshadowing a pivot in practice that might be “slow to start with”.
The CAVA (Central venous access devices for the delivery of systemic anticancer therapy) trial is a National Institute for Health Research- (NIHR-) funded open–label, multicentre, randomised controlled trial that compared complication rates and costs of the three devices used to deliver anticancer drugs via a central vein.
It is reported to be the largest randomised trial to date to compare all three devices, and set out to establish acceptability, clinical effectiveness, and cost-effectiveness of the devices for patients receiving SACT for three months, or more.
“The bottom line is, for a solid cancer, if you are going to need intravenous chemotherapy for three months or more, you should be offered the option of a PORT. We should try and empower patients so that that this will be something they think will be best for them,” Jonathan G Moss (Institute of Cardiovascular and Medical Sciences, Glasgow, UK), chief investigator, tells Interventional News on the subject of increased PORT take-up.
The paucity of good evidence comparing central venous access devices (CVADs) entails that neither the European Society of Medical Oncology nor the American Society of Clinical Oncology make specific recommendations regarding the type of device to be used.
CAVA showed that PORTs were associated with a reduction in complication rate of about 50% when compared to a PICC line, and when compared with the Hickman line. “There was a fairly strong preference for PORTs, amongst both the patients receiving them and also the healthcare staff who look after them. These were basically felt to be better devices and the only downside is the cost and whether these services are set up and geared to deliver these devices compared to the other two in a timely manner,” he added.
Resetting UK practice may not be a brisk business

Moss outlines that decision-making processes behind the choice of device are “poorly understood” globally. Eye-catchingly, PICC use has been captured to be buoyant. “PICC usage has increased over the past decade and is now the dominant strategy in many western European countries and the USA.” This spike in PICC popularity may be underpinned by the ease of insertion of these devices enabling prompt placement and removal by nurse-led teams, local availability of devices, technical issues such as the avoidance of the vital structures in the neck, and perceived lower up-front costs—but there is a sketchy evidence base behind this uptick, the authors say. “PORTs, by contrast, are the most expensive and least frequently used of the three devices,” Moss emphasises.
On stemming the tide of PICC use, the lead author continues: “Changing policy in institutions like the NHS [UK National Health Service] is never easy. There will be all sorts of reasons why people do not want to change—with costs being one and who is going to be putting in the PORTs [being another], and how quickly they can be put in. […] There are lots of nurse teams at the moment who have been trained to place PICC lines. We need to be able to sell the message to them that we are not saying they should not provide a service for patients but trying to persuade them to put in a different device. I think we need to try and move away from doctors putting in the PORTs and nurses putting in the PICC lines. These are all fairly straightforward procedures to place, and I have great confidence that we can empower nursing teams to place all three devices, but particularly PORTs.”
Moss acknowledges that the complication rates and costs of nurse-led teams placing PORTs was not tested by CAVA, but emphasises that most skill mix is not evidence-tested. “We did not compare different operator groups regarding complication rates as that was not the purpose of the trial. We do know the technical (or periprocedural) complication rates in CAVA were exceptionally low, reflecting well-trained staff using ultrasound guidance. Most of the complications related to these devices arise from their subsequent usage and maintenance. We simply do not have enough events to compare periprocedural complications across operator groups, and have no reason to believe that based on this very low complication rate, that any one group (nurses, anaesthetists or radiologists) was technically better than another. We continue to support the concept of nurse-led vascular access teams in order to make widespread practice change practical to deliver.”
The authors back the challenge “to change the service delivery model so that PORTs can be provided in a more timely and cost-effective manner. There will still be a small group in whom the other devices are preferred. Guidelines should be updated to reflect this new evidence,” they write.
They also probed the issue of cost, which is another factor that will play into service transformation. “We have got to persuade the people that pay for these, the managers, that although the PORT is more expensive at the shop front, at the end of the day, when you look at the total package of care [when dwell time is taken into account], that they actually are no more expensive, or a little bit cheaper. And again, that is sometimes difficult to sell in the NHS because we tend to focus on frontline costs,” explains Moss.
Four-way randomisation in CAVA
CAVA randomised patients with an algorithm taking into account centre, body-mass index, type of cancer, device history, and treatment mode. The trial included adults receiving SACT over a three-month or longer period for solid or haematological malignancy from 18 oncology units in the UK. There were four available randomisation options: Hickman vs. PICCs vs. PORTs (2:2:1), PICCs vs. Hickman (1:1), PORTs vs. Hickman (1:1), and PORTs vs. PICCs (1:1) and these then allowed three 2×2 comparisons, PICC vs. PORT, PICC vs. Hickman and PORT vs. Hickman to be made.
“The primary outcome was complication rate (composite of infection, venous thrombosis, pulmonary embolus, inability to aspirate blood, mechanical failure, and other) assessed until device removal, withdrawal from study, or one-year follow-up,” the authors report in The Lancet.
The triallists screened 2,714 individuals for eligibility, 1,061 were enrolled and randomly assigned (PICC vs Hickman n=424, 212 [50%] on PICC and 212 [50%] on Hickman; PORT vs Hickman n=556, 253 [46%] on PORT and 303 [54%] on Hickman; and PORT vs PICC n=346, 147 [42%] on PORT and 199 [58%] on PICC).
PORTs outpace other CVADs on nearly all fronts
Between 2013 and 2018, 1,061 patients were enrolled and randomly assigned (PICC vs. Hickman n=424, 212 [50%] on PICC and 212 [50%] on Hickman; PORT vs. Hickman n=556, 253 [46%] on PORT and 303 [54%] on Hickman; and PORT vs. PICC n=346, 147 [42%] on PORT and 199 [58%] on PICC).
- Similar complication rates were observed for PICCs (52%) and Hickman (49%).
- PORTs were superior to Hickman with a complication rate of 29% vs. 43%.
- PORTs were superior to PICCs with a complication rate of 32% vs. 47%
Painting a picture of the trial’s main findings, Moss and colleagues report: “There was little difference between PICCs and Hickman in terms of complications. CAVA showed that PORTs reduced the adverse event rate by approximately 50% compared with Hickman and PICCs. A device specific quality of life instrument showed no difference between PICCs and Hickman, but a preference for PORTs. PORTs were associated with the highest total costs; however, after allowing for the dwell time of the devices, there was no difference between PICCs and Hickman, but the cost associated with PORTs was lower when compared with PICCs and Hickman.”
See Moss’ views on the value of randomised controlled trial data: