
In February 2018, the first European case of endovascular aneurysm repair (EVAR) for the treatment of an abdominal aortic aneurysm was performed using a prototype device based on augmented reality by Nyali Swiss, an advisory company based in Lugano, Switzerland, write Anna Maria Lerardi, Mario Petrillo, Salvatore Alessio Angileri and Gianpaolo Carrafiello (pictured), from Milan, Italy.
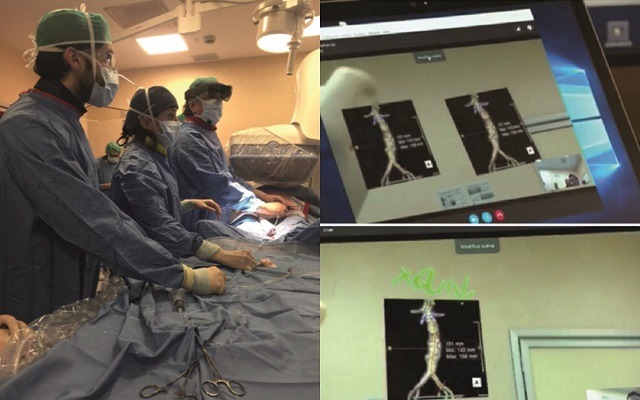
The procedure was performed in the angiosuite of San Paolo Hospital, in Milan, Italy. In real time, several doctors, residents and students, watched (via live streaming) the procedure above with “the eyes of the first operator”. The “spectators” were in Pisa, Italy, where the first edition of the European Campus in Interventional Radiology took place, dedicated to Italian and European residents.
The prototype device used is based on “space-cognizant” augmented reality that is able to superimpose virtual objects on the surroundings. The “virtual objects” represented in each scenario can have spatial relationships with real objects in 3D space: in our case an external operator was able to draw arrows or annotation on specific points on the patient’s skin or in other locations in the angiosuite.
The result was a strong interaction between the first operator, external consultants and the “spectators” in Pisa. All subjects were able to see and interact with the first operator.
In the meanwhile, the first operator was able to consult some virtual objects located in the angiosuite like the CT scan of the patient and some other documents that were able to help during the procedure. These were all superimposed as holograms in specific areas of his field of view.
Many start-ups are currently using augmented reality technologies for employee training: the aim is to familiarise trainees with different environments or specific scenarios. This approach is derived from the military, which has been experimenting in augmented reality interfaces for years.
It is now being exploited in interventional radiology to enable a consultant to virtually (outside of the operating theatre, at home or anywhere in the world) make suggestions to the first operator to decide on strategies, or issue warnings that are useful for the correct execution of the treatment by sharing the same field of view and the same information. In more and more cases, non expert operators may deal with challenging situations by calling upon help “from home”. This could be a more expert colleague (at home; in another room; or somewhere else in the world entirely) who is now able to see the procedure and suggest real-time operating strategies.
Our experience could be considered a milestone in augmented reality applied to interventional radiology, switching as we were from a virtual scenario to the patient bedside.
We have observed a faster learning curve for novice operators compared with the usual coaching when we have used augmented reality. More students, residents and interested physicians may follow the procedure from outside the operating room.
Our aim is to use augmented reality to help manage the pain and distress associated with a wide variety of interventional radiology procedures by using different strategies focused on integrating analgesia with anxiety reduction. To this end, patients can wear special glasses equipped with immersive virtual reality and dial up a scene from a beach or any other different relaxing scenarios during different interventional procedures (whether they are oncological or not). The aim is to investigate and capture the compliance and experience of patients with and without glasses.
In our department, we routinely perform percutaneous thermal ablation of solid tumours under mild sedation that provides both analgesia and anxiety reduction. We have undertaken a study that was based on the premise that virtual reality glasses can serve to “distract” the patient from the pain of the procedure and preliminary results are showing that a lower dose of benzodiazepine was used in patients who wore glasses. We are also performing the same investigation in a non oncological setting, specifically in the context of interventions to treat low back pain. Every year, we treat almost 200 patients with percutaneous lumbar and cervical disc decompression and our idea is to compare the dose of analgesics administered in patients wearing virtual reality glasses with those who do not. Moreover, a questionnaire to investigate patient compliance during the procedure will be proposed to every patient.
Virtual and augmented reality are new, evolving fields with several applications that need testing in clinic in order to help the technology mature and go beyond just entertainment.
Anna Maria Lerardi, Mario Petrillo, Salvatore Alessio Angileri and Gianpaolo Carrafiello (professor and chief of Diagnostic and Interventional Radiology Unit) are from the University of Milan, Milan, Italy.










