
This advertorial is sponsored by Argon Medical.
Danial Jilani is an interventional radiologist based at Northwestern Medicine Palos Hospital (Chicago, USA), who uses the SKATER™ drainage catheter (Argon Medical) as his “go-to” catheter for a range of both “bread and butter” and more complex interventional radiology (IR) procedures. He spoke to Interventional News about why SKATER works so well for him and his patients, and the findings of a recent bench test that compared SKATER to other percutaneous drainage catheters on the market.
For Jilani, SKATER’s “all-purpose” suitability means he can use it for pneumothoraxes, chest tubes, pleural effusions, nephrostomy and biliary procedures. Moreover, SKATER works for sclerotherapy too. Ethyl alcohol and doxycycline used in this type of treatment can “break certain catheters down”, Jilani explains, however SKATER “can tolerate both these agents—having the luxury to handle both is one of the advantages of this catheter.”
There are multiple “subtle differences” that set SKATER apart, Jilani goes on to tell Interventional News. The recent findings of a bench test1, which compared a range of percutaneous drainage catheters on the points of kink resistance, flow rate and ‘pushability’ shed light on these, he reports. Among those tested, SKATER, made of a blend of durable polyurethane material, was found to be the most kink-resistant, in turn improving flow rate. Jilani notes that SKATER demonstrated a high flow rate during the bench test, with 8Fr catheters and mini pigtail catheter loops—in spite of their small size, which would typically reduce flow rate. The large, skived holes are one of the features that allow for maximal drainage.
Jilani then speaks to the ‘intrinsic mechanisms’ of SKATER that, in the bench test, helped it fare more favourably than other drainage catheters. One was the “locking shoulder tip, which decreases buckling during insertion.” The hydrophilic coating also reduces friction as it is being inserted. The force required to insert the SKATER was 22% less than for some of the other catheters, and 70% less with the mini-loop catheter, Jilani relays, opining that this is an “underrated” feature of drainage catheters across the board.¹
Case study 1: Nephrostomy tube placement for malignant obstruction
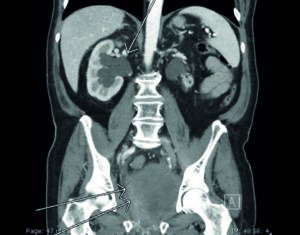

Citing a further benefit of using SKATER, Jilani goes on to elucidate how the position markers on the SKATER are “especially helpful when doing a procedure under CT [computed tomography] guidance, as you are stepping in and out of the room and do not have your hands on the catheter the whole time”. Precision, as facilitated by these markers, is key as in a few millimetres “you can be in a structure you do not want to be in,” Jilani elaborates.
In addition, the low-profile locking system SKATER offers is, Jilani says, “so easy to use that I was able to teach myself [how to use it]”. Providing anecdotal context for these positive data, Jilani then explains how inserting a drainage catheter into a cirrhotic liver can feel like “pushing up against a rock”, making buckling more likely. Hence, SKATER’s proven ‘pushability’ is advantageous. “The more difficulty you have [overall] during the case, the more things can go wrong and the more time the patient spends on the table,” Jilani admits, suggesting a further reason why having a drainage catheter that can perform as SKATER did in the bench test, across all the aspects assessed, is beneficial.
Case study 2: Chest tube placement for spontaneous pneumothorax in patient with COPD
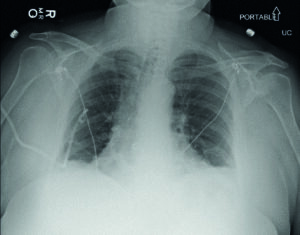

Jilani goes into detail about how using SKATER can yield advantages for patients and their outcomes—“I am a firm believer that the faster you can drain an abscess, the less risk there is of recurrence.” Chronic abscesses can last for months, which, in turn, requires long-term drainage. However, with SKATER’s “large skived holes and fast flow rates”, catheter drainage is more efficient. “For the majority of patients with abscesses, we place these [SKATER] catheters and within a week, we can remove it, sometimes even faster,” Jilani relays.
Inadequate flow rate, such as seen in other types of catheters that kink more readily, means drainage takes longer, Jilani reiterates. “We follow our patients closely,” he asserts, meaning that he can say with some confidence that he has noticed “far fewer instances of kinking” compared to earlier in his career when he used other drainage catheters. Longer drainage time can lead to occlusion from bacteria and fibrin build-up and more catheter exchanges, prolonging the overall time the patient has a catheter in. Even without complications, Jilani explains that having a drainage catheter in for a long time is “very inconvenient” for patients—“they are attached to a bag […] which can make day-to-day activities hard.”
Case study 3: Percutaneous drainage of infected bladder/acute cholecystitis
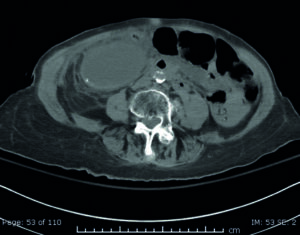

The improved patient outcomes—faster drainage and therefore fewer complications related to chronic abscesses and catheterisation—that SKATER facilitates, reduce healthcare costs, Jilani is also keen to acknowledge.
To round off the discussion, Jilani summarises what it is about SKATER that makes it his “go-to” drainage catheter. “The subtle differences make an impact,” he states, referring back to SKATER’s high level of performance in the bench test: for kink resistance, flow rate and ‘pushability’. The evidence the test produced supports Jilani’s own clinical experience that “[the SKATER catheter] works well and is associated with better patient outcomes”, meaning he can continue to use it with confidence.
References: 1. Data on File. Bench Testing Comparative Data Relative to Drainage Catheter Performance: An analysis of pigtail drainage catheter systems.









