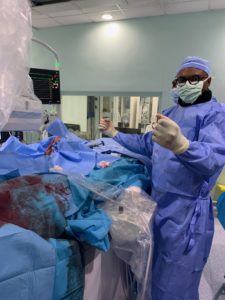
There are fewer than five practicing interventional radiologists in Nigeria today, a country of 200 million people. Hammed Ninalowo aims to change that ratio, founding the organisation IRDOCNIGERIA, with the aim of training an additional 100 interventional radiologists in his home country over the next decade. Having trained in the USA, Ninalowo describes the experience of performing the first ever transjugular intrahepatic portosystemic shunt (TIPS) in sub-Saharan Africa, and looks forward to the launch of the first interventional radiology training programme in the country in September this year.
When I told my colleagues in America that I was considering performing a transjugular intrahepatic portosystemic shunt (TIPS or DIPS: direct intrahepatic portosystemic shunt) on a Budd Chiari patient in Nigeria (see image below), most said I was crazy. But I remember thinking, “If I do not do this, who will?”. After extensive planning from myself and my team, we were able to pull the procedure off with an amazing clinical outcome. A 20-year-old woman who had had 33 litres of ascites drained from her body over the last three years at monthly intervals and had lost all muscle mass now has no ascites, has regained muscle mass, and is returning to school.
My story of practising interventional radiology in Nigeria did not start there, however. Pulling off the first TIPS/DIPS in sub-Saharan Africa is just a small fraction of our journey.
I was born and raised in Lagos, Nigeria, and left in 1999 to pursue an education, though I always had a homeward focus. I finished by Bachelors degree in 2003 and graduated medical school in 2010. While in medical school, I continued to look back to Nigeria, and spent the summer of my first year at a teaching hospital in Lagos. My guiding principle all through medical school regarding specialty and career choice remained “What can I bring back to my people?”. I was involved in the care of a patient in the intensive care unit in my third year of medical school; he had undergone two endoscopies due to bleeding varices, yet continued to bleed. An interventional radiologist was called in and, through just a tiny hole in the neck, placed a stent graft and coiled off varices, triggering an immediate change in the patient’s haemodynamics. That was it. My specialty was chosen and my interventional radiology journey started.
I trained in diagnostic radiology at the University of Maryland. My mentors always asked me what my future plans were, and it always circled back to what I planned to do in Nigeria. I took multiple trips to Nigeria during training to survey the state of medicine and also visited some of the local pioneers who had made a move back home in fields like interventional cardiology and changed the narrative as to what was possible locally. I went on to finish subspecialty training in interventional radiology at the University of Pennsylvania. I have since worked in a large hospital system in Pennsylvania (Geisinger health system), a tertiary care centre with level one trauma and multiple transplant programmes.
In early 2018, I was ready to make my push into Nigeria and heard of a group in Nigeria called the Nigerian Society of Interventional Radiology (NiSIR). I learned this group was attending the Pan Arab Interventional Radiology (PAIRS) meeting in Dubai. I immediately bought a ticket. I met many bright minds, mostly working in the public sector, who had left the country to obtain training and were back in Nigeria providing amazing care to patients. However, there were significant frustrations, as they had not been able to open all the possibilities offered by interventional radiology in the public sector. One of these gentlemen was Professor Ahmed Ahidjo, now the Chief Medical Officer of the University of Maiduguri, who I still credit as the real pioneer of interventional radiology in Nigeria. I knew I had trained at one of the best IR programmes in the USA and had been lucky enough to work and gain experience in a high volume complex practice. I was ready to make my push.
I initially started by collaborating with the public sector—however, it was immediately apparent that the resources there were significantly limited, and getting things done in the government hospitals was a difficult task. I immediately changed my goals to: 1) Look for a progressive organisation that believed interventional radiology was possible in Nigeria and work hard to show what is possible at a complex level immediately providing care to patients; 2) Continue to collaborate with the public sector to create sustainability in the country. With these objectives, I founded IRDOCNIGERIA, a company providing IR services in Nigeria, and started the IR division of RAD-AID international Nigeria.
Since our first case in September 2018, we have completed many complex procedures, including complex venous recanalisations, TIPS/DIPS, transarterial chemoembolizatons (TACE), varicocele embolizations, uterine fibroid embolizations (UFE), biliary stenting and recanalisation for chronic total occlusions using SAFARI, to name a few. We now offer any procedure in interventional radiology except for radioembolization. In September this year, we are hosting a symposium at the University College Ibadan with several SIR Faculty members, and we will launch the first training programme in Nigeria.
Achieving this has not been easy. The time spent across two continents has been a challenge—though the greatest challenge remains the supply chain for interventional radiology in sub-Saharan Africa and the infrastructure in public institutions. It is no secret that interventional radiology consumables are not cheap, but the cost is a minor factor, as most manufacturers (except currently Medtronic) do not do business in Nigeria or many African countries. There is something interesting going on with a lot of African economies; many markets have emerged in the last few decades, and with this, modern medicine is on the rise. African patients spend an incredible amount of money on medical tourism to places like India and the West. In a very small way, I have stopped a few patients from making these trips. We can keep and treat these patients in Africa and keep the money in Africa for Africa. It will require some sacrifice from the industry, but most of the sacrifice will have to be made by Nigerian physicians in the diaspora who have acquired a significant amount of knowledge and thrive in most of their chosen fields. I say the days of “Tent medicine and medical missions” are dying, as these do not create sustainability. We need to improve the long-term state of healthcare in these countries by focusing on people and services who are committed to full time or long term sustainability driven projects.

For me, I have simply been on a mission and I have not looked back. I can say with authority that the future of medicine, on any continent, without interventional radiology is no future at all. My goal in the short term is to transition my practice full time to Nigeria, an ambition well known to those around me. A colleague in Nigeria uses the phrase #TheNigerianPatientsAreWorthIt, and I agree. Our journey has just started, but watch this space, as I am committed not only to Nigeria, but to collaborating across Africa to bring the life saving minimally invasive procedures of interventional radiology to the continent at large.
Hammed Ninalowo is an interventional radiologist in Lagos, Nigeria.











Great vision sir. May the intent of this be in Jesus name. Amen
Very, very well done, Hammed. Proud of you!
Very nice work
welcome to Tanzania having the same efforts through road2ir we can join our efforts so that we speed up the outcome
Be blessed
Well done Hammed!!!!
Like Douglas Okor says, The Nigerian Patients Are Worth It……Well done
Well done Hameed. Nigerian patients are truly worth it.
well
Well done Hammed and may God bless you with the wisdom to make interventional a reality in all parts of the country. The challenges in IR are enormous despite the abundant interest by young radiologist in Nigeria . We currently have no centre for IR subspecialisation in Nigeria. Oversea sponsorship are nonexistent. The best we could do in my centre (UUTH) is send a colleague to Ghana and hope to learn from him when he is back. Even when he comes back, there are no available facilities to put to practice what he has acquired. I hope to have opportunity to learn from guys like you who remember to contribute their knowledge for the betterment of their country. Wishing you success.
Excellent work
Keep up the good work! Thanks for making a difference.
Wonderful news! Great job, Dr Hammed…. What a selfless driven aspiration. For thinking of this & going ahead with your vision, radiologists like me are very happy to associate with you. Please let us know how we can key into this vision..the more of us trained to do IR cases, the faster your vision will be achieved.
We need to think beyond ourselves, our future can only be brighter, when the common good of all, becomes paramount.
Well done, Sir & God bless you.
This is phenomenal!….making this leap of faith back home this early in your career rather than waiting till you retire in the U.S. and come back when all this vibrance of youth is almost gone. God bless your efforts immensely! I still firmly believe Nigeria has hope for that bright light at the end of its tunnel. Please, keep up the good work!
…Judith A. Ogoh, R.Ph., Pharm.D. Texas…also moved home and trying to make a difference in the Pharmacy world!
Thanks for believing in Project Nigeria.People like you inspire us to keep hoping and keep believing.
Great work. I am pleased to be associated with you
Nice one Hammed!.. Super proud of you!!
Good stuff but missing vital information. What is the contact phone and email for Dr. Ninalowo.
Dr Ninalowo Hammed is a true and selfless Nigerian doctor. He is going to inspire many radiologists to go into IR which i have always loved and desire to gain more experience in. Sir, may your vision and mission for our dear fathers land never fail.
I JUST MET YOU IN PERSON TODAY, AND IT IS MORE INSIGHTFUL READING THIS. THANKS DR NINOLOWO, NIGERIANSANDAFRICANPATIENTSTRULYWORTHIT.
NURSE TEMIDAYO MICHAEL. ABUJA.
Wow, this is good, I wish we have more like you, God bless your selflessness
Very well done Dr. Hammed. I would like to talk about your performance in my page @interRadiologia. I am a Spaniard Special Procedure Technologist in Interventional Radiology. Please, keep your faith and good work up, and make your dream become true 🖖☢️💪🏽
Dr Jammed…great feat you have made already at a young age. You sure inspire me and a whole lot of us. Keep up the good work.
This makes my interventional radiologist dreams come to reality sir reach your goal sir and I’ll like to train with you
It’s a good thing to have come across your story. I am also starting my journey in Radiology. I’d be pleased to be your mentee. I desire interventional radiology as well.