
With an increasing number of interventional radiologists turning their technical and clinical expertise to musculoskeletal embolization, Sandeep Bagla and Abin Sajan believe it is important to have a thorough understanding of the anatomy specific to these procedures. Here, they detail the genicular artery anatomy, in the hope that increased physician familiarity translates into an increased ability to treat patients with challenging vasculature.
In an era of cutting-edge interventional procedures, genicular artery embolization (GAE) is a minimally invasive solution for patients with mild to moderate osteoarthritic (OA) knee pain. The primary goal of GAE is to disrupt the inflammatory process by embolizing the hypervascular synovium causing the pain and disability. Successful preliminary results in pilot clinical studies have fostered a randomised control trial (RCT) at the Vascular Institute of Virginia and UNC Chapel Hill, which has finished recruitment and we hope to present our findings at the annual meeting of the Society of Interventional Radiology (SIR) next year (28 March–2 April, Seattle, USA).
As the popularity of GAE increases, it is important to have a thorough understanding of the genicular arterial anatomy. The success of GAE, as well as the prevention of non-target embolization, is associated with recognising patterns on the initial angiogram and anticipating potential obstacles during the procedure. Possible anatomic challenges include variable presence of vessels, small sized vessels, acutely angled vessel origin, presence of atherosclerosis, and collateral supply. Familiarity with typical patterns and an understanding of angiographic relationships provide a dynamic foundation when presented with challenging anatomy.
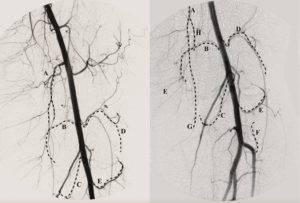
We reviewed the angiographic patterns from our first two clinical trials to identify the basic arterial anatomy and review technical pearls for the procedure. We identified six main arteries: descending genicular artery (DGA), medial superior genicular artery (MSGA), medial inferior genicular artery (MIGA), lateral superior genicular artery (LSGA), lateral inferior genicular artery (LIGA), and anterior tibial recurrent artery (ATR). Since osteoarthritic knee pain can be lateralised to either the medial or lateral aspect of the knee, we present the anatomy using the same approach (Figure 1). Of note, other vessels, including the median genicular artery, contribute to the knee joint but were not included in our study.
The medial compartment of the knee is mainly perfused by the DGA, MSGA, and MIGA. The DGA originates from the distal superficial femoral artery and has a classic inverted “Y” appearance. It divides into a straight medial saphenous branch which courses superficially, and a more torturous lateral musculoarticular branch which courses deeper in the knee.
The MSGA arises from the proximal-mid popliteal artery just above the medial femoral condyle and classically courses superiorly before travelling down to the medial knee joint. Although the MSGA is often difficult to visualise given its smaller calibre, we have noted that the luminal size of the MSGA is inversely related to the size of the DGA. The MIGA originates from the popliteal artery near the joint space and descends along the upper margin of the popliteus, before coursing anteriorly and superiorly, creating an angiographic “V” around the medial tibial condyle. The MIGA arises adjacent to the sural arteries, which are distinguished by their steeper trajectory towards the gastrocnemius musculature.
The lateral compartment of the knee is mainly perfused by the LSGA, LIGA, and ATR. The LSGA arises from the mid-popliteal artery at the level of the lateral femoral condyle. Like the MSGA, it initially courses superolateral before travelling down to the lateral knee joint. The LIGA originates around the joint space and courses laterally above the fibular head before wrapping around the lateral tibial condyle, creating a “J” appearance. In addition, this reversecurved vessel may share a common trunk with the SMGA, making catheterisation more challenging. The ATR is the most inferior branch supplying the knee and originates from the very anterior tibial artery just beyond its origin.
Although the six arteries are typically present in all patients, absence of one or more arteries might suggest that another artery is more dominant in the affected compartment. Additionally, collateral supply can cross the joint space and embolizing in such cases can lead to non-target embolization of the asymptomatic side. Cutaneous branches often appear perpendicular to the main genicular artery and terminate at the skin surface. Skin purpura from embolizing these vessels is the most common side effect of GAE, and an attempt should be made to deliver particles distal to cutaneous branches, however this may be challenging given their ubiquitous presence. Ice-packs placed on the skin may minimise the risk of non-target related cutaneous changes.
The most technically challenging aspect of GAE is catheterising the acutely angled vessel origins (Figure 2). Wire placement can be challenging in the first 3cm, and wires with a floppy tip may not allow ample support during catheterisation. In our experience, a 2.4F microcatheter was adequate in catheterising these arteries. However, there is a role for pre-shaped microcatheters, especially in acutely angled vessel origins, most notably the SMGA and the SLGA.
GAE is an exciting procedure that is leading the way for musculoskeletal embolization. We believe that a thorough understanding of the angiographic anatomy and knowledge of commonly encountered challenges will increase interest in GAE and promote future cutting-edge interventional procedures.
Sandeep Bagla is the chair of Interventional Radiology at the Vascular Institute at Virginia, Woodbridge, USA. For his GAE clinical studies, Rachel Piechowiak and Ari Isaacson are coinvestigators.
Abin Sajan is a medical student at the State University of New York (SUNY) Downstate College of Medicine, New York, USA. He was awarded the SIR Dr and Mrs WC Culp Student Research Grant for his work on the “Cadaveric Classification of the Geniculate Artery Anatomy”. He is working with Maziar Sighary on the cadaveric studies.











