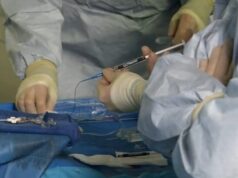
A large US nationwide study shows that the uterine fibroid embolization is vastly underutilised, compared to hysterectomy—especially in rural and smaller hospitals.
In fact, there were more than 65 times as many hysterectomies performed than embolizations, despite data showing that the minimally invasive procedure results in substantially lower costs and shorter hospital stays than the surgical option, the study reveals.
The research was presented today at the Society of Interventional Radiology’s 2017 annual scientific meeting (4–9 March, Washington, DC, USA).
“These findings suggest there is a lack of awareness about this safe, effective and less invasive therapy for uterine fibroids,” said Prasoon Mohan, the study’s lead author and assistant professor in the Department of Interventional Radiology, University of Miami Leonard M Miller School of Medicine, Miami, USA.
“Interventional radiologists urge healthcare professionals to present patients with all available treatment options so that the patient can make an informed decision. Patients need to know about the major differences between surgical treatments and uterine fibroid embolization, especially that this is a non-surgical treatment that preserves the uterus and has a much faster recovery time compared to hysterectomy.”
According to the National Institutes of Health, a majority of women—almost three out of four—will develop uterine fibroids by the age of 50. Women are at increased risk for developing fibroids if they are overweight, African-American, over the age of 40, have high blood pressure, have had no children, and have first-degree relatives with fibroids.
Fibroids develop from the uterine muscular wall and vary in size from a quarter of an inch to larger than a cantaloupe. In most cases, women are not aware that they have fibroids because they do not have symptoms. Symptoms when they occur include heavy menstrual bleeding, pelvic pressure or pain, abdominal enlargement, pain with intercourse, constipation and frequent urination.
This study included an analysis of data from the 2012 and 2013 Nationwide Inpatient Sample (NIS), the largest all-payer inpatient healthcare database in the country. Using billing codes that identified hysterectomies and embolizations completed for the treatment of uterine fibroids, researchers compared how women were treated for this condition, the costs of the treatments, and the outcomes.
The data revealed that over this period, 165,000 more hysterectomies were performed than embolizations (167,650 vs. 2,470, respectively) nationwide. Further, researchers found that only 0.4% of fibroid embolizations were performed in rural hospitals compared to 9.4% of hysterectomies in the same setting; and 7.9% of embolizations were performed in small hospital systems compared to 67.4% in large hospital systems.
“The fact that so few women undergo uterine fibroid embolization in rural and small hospital settings shows a healthcare access and education disparity in who receives this treatment. It is important that we continue to educate patients about choice and determine ways to increase access to this effective, less invasive therapy,” said Mohan.
The data also showed that embolization resulted in shorter hospital stays (2.16 for vs. 2.32 days), and was less expensive than a hysterectomy by about US$12,000 (US$21,583 vs. US$33,104). Further, the women who elected to undergo embolization had more chronic conditions than found in the patients who received a hysterectomy.