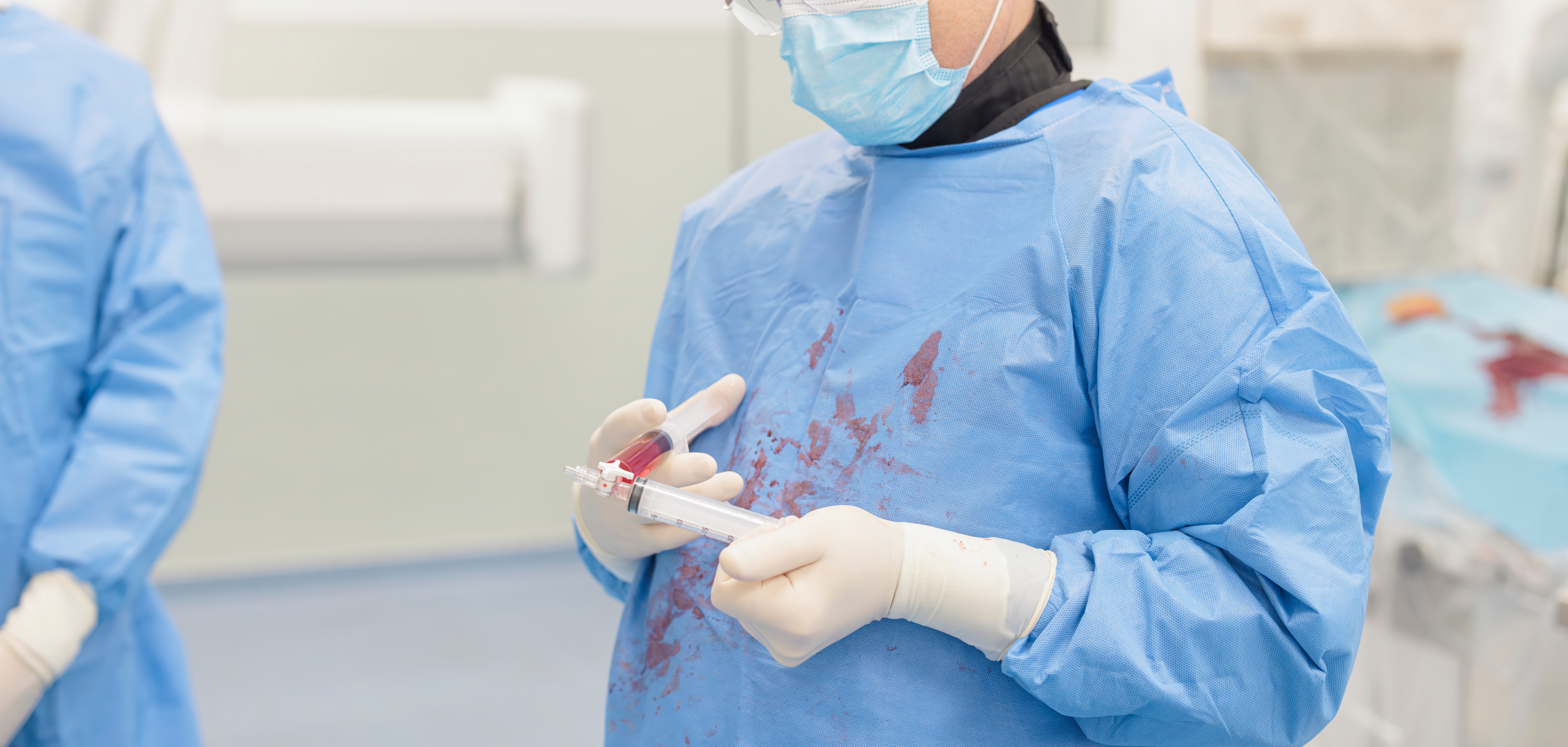
 Nine medical societies are calling for updated safety standards in fluoroscopy laboratories, where clinicians face radiation exposure and orthopaedic injuries from heavy protective equipment.
Nine medical societies are calling for updated safety standards in fluoroscopy laboratories, where clinicians face radiation exposure and orthopaedic injuries from heavy protective equipment.
A report published simultaneously today in JSCAI, Heart Rhythm, JVIR, and JVS–Vascular Insights details the health, financial, and workforce impacts of fluoroscopy-guided settings and proposes an enhanced safety framework: ALARA+—meaning As Low and As Light as Reasonably Achievable.
Read the report: ALARA+: Summit on Radiation and Orthopedic Risks in Fluoroscopic Laboratories
The report addresses the dual occupational hazards linked to fluoroscopic procedures—radiation exposure and orthopaedic strain from traditional protective equipment—and aims to ensure that safety is built into the environment, equipment, and standard of care.
“How we think about radiation safety has been historically guided by the ALARA principle, or ‘as low as reasonably achievable.’ But that approach has proven to be not safe enough for healthcare staff working in fluoroscopic labs,” said Robert F Riley (The Christ Hospital, Cincinnati, USA), chair of the 2025 Summit on Radiation and Orthopedic Risks in Fluoroscopic Labs. “Traditional ALARA principles focused on incomplete methods of minimising radiation exposure. Additionally, they did not fully account for the orthopaedic strain caused by wearing heavy lead protective equipment during long procedures. The new framework, ALARA+, calls for responsible protection strategies that are ‘as low and as light as reasonably achievable’ for the entire team.”
ALARA+: Summit on Radiation and Orthopedic Risks in Fluoroscopic Laboratories is endorsed by the Society for Cardiovascular Angiography and Interventions (SCAI), American College of Cardiology (ACC), Alliance for Cardiovascular Professionals (ACVP), American Society of Echocardiography (ASE), Heart Rhythm Society (HRS), Society of Interventional Radiology (SIR), Society of NeuroInterventional Surgery (SNIS), Society of Vascular and Interventional Neurology (SVIN), and the Society for Vascular Surgery (SVS).
Fluoroscopy is widely used to perform minimally invasive procedures that treat conditions such as heart attack, stroke, and vascular disease. Using real-time X-ray imaging, clinicians guide catheters and other devices through blood vessels to diagnose and treat disease without open surgery.
While these procedures improve patient outcomes and shorten recovery times, they carry long-term occupational risks for the teams performing them, as they receive thousands of low but repeated radiation doses over the course of their career. To reduce exposure, clinicians often wear heavy lead or lead-equivalent protective garments that can weigh 15 to 20 pounds. However, the strain of wearing them during long procedures contributes to chronic neck, back, and joint injuries.
“These occupational harms affect every member of the procedural team and the healthcare system as a whole, carrying major financial and human costs,” said summit co-chair Arnold H Seto (Long Beach VA Medical Center, Long Beach, USA). “Across fluoroscopy laboratories, clinicians and staff face both cumulative radiation exposure and the physical burden of heavy protective equipment. Over time, that means years of strain from protective gear and nonergonomic lab setups. The consequences are real. People develop chronic pain, require surgery, and some are left with severe spinal conditions that limit or even end their procedural careers. Maintaining a skilled workforce in these labs, which is already in limited supply, is essential to ensuring patients have access to these lifesaving procedures. As demand for minimally invasive procedures continues to grow, protecting and retaining experienced teams will be critical to preserving and expanding access to care.”
A 2023 Occupational Health Hazards Survey from SCAI found that roughly two-thirds of interventional cardiologists report musculoskeletal pain related to working in the cath lab or wearing radiation protection equipment. These risks affect the entire procedural team, including physicians, nurses, technologists, and imaging specialists. Trainees may accumulate higher exposure near the radiation source while developing procedural skills. Concerns about radiation exposure during pregnancy and the physical burden of protective lead are often cited as discouraging many women from entering or remaining in fluoroscopy-based specialties.
To address these risks, the multi-society summit report calls for several actions to improve safety in fluoroscopy laboratories, including:
- Accelerating the adoption of modern radiation protection technologies, such as suspended, freestanding, or table-mounted shielding systems that reduce exposure without requiring clinicians to wear heavy protective garments
- Expanding real-time radiation monitoring to enable clinicians to receive immediate feedback and reduce exposure during procedures.
- Strengthening education and training in radiation safety and exposure reduction for physicians, trainees, nurses, and technologists.
- Continuing technological innovation to protect all catheterisation lab clinicians.
- Supporting regulatory and accreditation standards that promote safer fluoroscopy laboratory environments.
“ALARA+ represents a shift from accepting risk to expecting better,” said SCAI president Srihari S. Naidu (Westchester Medical Center, Valhalla, USA). “Fluoroscopy-guided procedures save lives every day by allowing minimally invasive treatment for heart disease, vascular disease, and stroke. The clinicians and teams delivering that care deserve laboratories that protect them just as thoughtfully as we protect our patients.
“This multi-society call to action is about modernising safety expectations, not creating new obligations. We are calling for the acceleration of practical changes in technology, policy, and laboratory design so radiation exposure is minimised, and the physical toll of protective equipment is no longer treated as inevitable.”